Casebook: Common skin presentations in the elderly
Key points
- Venous eczema is often misdiagnosed as cellulitis
- Cellulitis is unlikely to affect both shins at once and tends to have a faster onset than venous eczema
- The management of venous eczema involves emollients, topical steroids and the promotion of venous drainage
- Ensure that an ankle-brachial pressure index (ABPI) is measured before applying compression to exclude arterial insufficiency – a reading between 0.8 and 1.3 is considered safe for compression
- In pruritus with no rash, when the clinical history and examination does not identify a cause, further investigation is warranted as underlying health conditions can contribute to or even cause pruritus in 20-30% of cases
- Note that approximately half of affected patients with pruritus and no rash will have no clear cause – this is idiopathic pruritus
Dr Tommaso Dazzi is a GP in Bristol
Case 1: Red shins
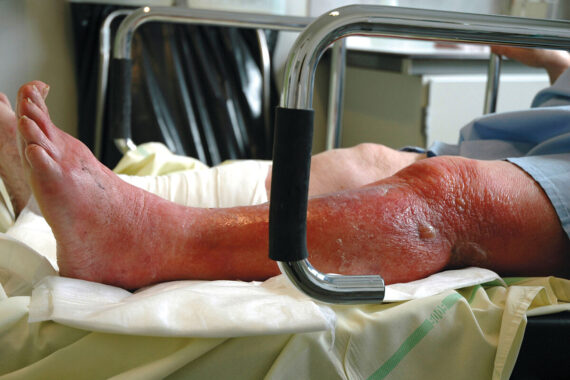
A 76-year-old lady presents with a two-week history of a red itchy rash around the gaiter area (lower third of the calf). She is accompanied by her daughter, who is worried about infection; in the past six months, she has noticed both ankles have become more swollen and her mother is generally more tired, short of breath and ‘not herself’.
What further questions should we ask?
There are three main aspects to consider:
Systemic symptoms Comorbidity can be a challenge in diagnosing presentations of red shins. Often there can be clinical overlap with multiple pathologies. This patient has been fatigued, short of breath and has swollen ankles. Causes of pitting oedema or lymphoedema should be investigated to rule out systemic disease. Oedema of the shins can itself cause skin stretching, pain and make the skin susceptible to infections or acute dermatitis.
Duration A short history – of days – may indicate a rapidly evolving pathological process such as an infection, for example cellulitis, but dermatitis (a term used to describe an inflamed or irritated epidermis) can also appear quickly. For this reason, dermatitis is often incorrectly treated as cellulitis. Dermatitis (a term used interchangeably with the term eczema) may be caused by sensitivity to allergens (as in allergic contact dermatitis), irritants (irritant contact dermatitis), genetic factors (atopic eczema) or chronic inflammation (as in venous eczema).
Location Cellulitis is unlikely to occur on both shins at once. In true cellulitis, if the foot is also affected, this may be a ‘tracking’ cellulitis – visibly extending along the lymph ducts. A common cause of cellulitis is skin breakdown in the foot’s web spaces with increased fungal and bacterial overgrowth, due to extended wear of damp or sweaty slippers. Erythema around the gaiter area is likely to be caused by lipodermatosclerosis and chronic venous disease. However, this is also a common location for erysipelas infection. Erysipelas is a more superficial skin infection than cellulitis, usually caused by streptococci. Compared with cellulitis, it has a more clearly demarcated erythematous edge, with a marked raised border, and unlike cellulitis, it may cause blistering.
The diagnosis in this case is not immediately apparent. This highlights the difficulty in diagnosing red shins in the elderly as the aetiology is often multifactorial. The presence of ankle swelling could demonstrate an underlying systemic disease such as heart failure, but the red rash in the gaiter area is often caused by venous eczema.
Click here to read the full article and download your certificate logging 2 CPD hours towards revalidation
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.









