I’m a GP who spent 150 days in hospital with Covid
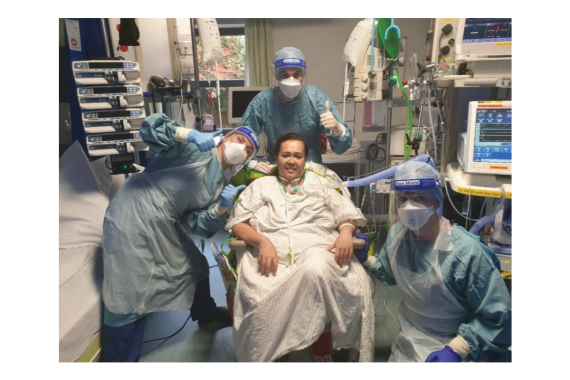
Just weeks after her 40th birthday, Dr Anushua Gupta found herself fighting for her life on a ventilator. A year on, she reflects on her remarkable recovery
Recently, I marked a bittersweet anniversary – one year since the start of my experience with severe Covid-19.
I’m a Manchester-based GP and I contracted the virus last March, just after celebrating my 40th birthday.
It’s difficult for anyone to say whether they contracted Covid at work. However, working on the front line put me in a high-risk category, especially at that time when there was no strict guidance on PPE or social distancing.
Looking back, some aspects remain etched in the memory. I remember the night I deteriorated, 4 April, like it was yesterday – I became severely breathless and started seeing a black winged figure. Immediately, I thought it was the angel of death, and was petrified.
With my oxygen saturations in the low eighties, an intensive care consultant told me I’d have to go onto a ventilator. I felt my worst fears were coming true – I asked my husband Ankur, a fellow GP, to show me our 18-month-old daughter Ariana on video. I thought I’d never get to see her again, or fulfil the dream we had of living into our eighties or nineties together. But I knew I had to keep it together for his sake; he had to be strong for Ariana, as I believed at the time that I was never going to come back.
Later that night, I was intubated, ventilated and put into a medically induced coma, where I stayed for around two months.
But despite this full support, I deteriorated further after 10 days. On 13 April, my team decided I’d have to go on ECMO (extra corporeal membrane oxygenation), to give me any chance of survival. I was one of the very few in the UK to go on ECMO for Covid at the time, and doctors had little, if any, hope that I would survive.
Finally, though, in mid-May I started to show signs of improvement. I went on to have a tracheostomy, and to be slowly weaned off sedation. However, I remained on the ventilator for a further eight weeks.
In July, I moved to the North West Ventilation Unit at Wythenshawe Hospital, where intense rehabilitation was integral to optimising my physical and mental health. Having gone through this scale of trauma, knowing how close I came to death and being away from my family and unable to hold my baby, I’d developed significant anxiety.
There were some complications after coming off sedation. It took me almost two months to muster the physical and mental strength to pull myself up from sitting and a further few weeks to take my first few steps. Intense physiotherapy is so important post-critical care. Doctors and nurses have told me that it was nothing short of a miracle that I survived.
I also wouldn’t have been able to recover as I did without the support from the speech therapy teams. Initially, my voice quality was just a whisper, and I was worried about it normalising, especially as around 80% of a GP’s job revolves around talking, whether with patients or colleagues.
I was finally discharged after 150 days, on 1 September, and since then, my rehabilitation has been exponential, with my daughter being my driving force.
I resumed working remotely in general practice in November, after only two-and-a-half months at home, which was really important to me – getting back into it felt like a step back to normal. I think a lot of people delay getting back to work, and that can work both ways. You do need to process what’s happened, but at the same time you need balance. I felt that was the right time for me to return, and it’s really helped with my recovery.
There were concerns about how long I could work for, so I only did short hours before my voice got painful, but my colleagues have been so supportive.
My recovery is by no means complete, but my problems are improving as I get more active, and my mental health is so much better. I try to keep a positive outlook, and feel I’ve been given a second chance in life. The power of supportive family and friends is phenomenal for mental and physical wellbeing.
I have so many thank yous, but the brilliant ECMO team at Wythenshawe, from director Dr Julian Barker to the doctors and nurses whom I didn’t get to know due to being sedated when under their care, saved my life, and I’ll be forever grateful to them, as well as to the AICU and NWVU doctors and nurses.
I am fundraising to help Wythenshawe AICU buy vital equipment, and I welcome contributions from Pulse readers.
Dr Anushua Gupta is a GP in Greater Manchester
To contribute to Dr Gupta’s fundrasing, visit justgiving.com/fundraising/anushua-gupta
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Related Articles
READERS' COMMENTS [6]
Please note, only GPs are permitted to add comments to articles










Thank you for sharing your story.
I am so glad you are making a gradual recovery and hope there few invisible scars.
Much love to you and your lovely little family
Great effort. Great news exists.
Inspirational story, thank you for sharing x
Incredible
This is a hugely moving account of the human impact of this horrible disease on someone who has dedicated her life to helping others as a GP. We are so lucky to have people like her in the NHS and even more so to have the back-up of our colleagues in the hospital who have saved so many lives. Thank you for sharing your story and good luck with the second phase of your life!
Well done Anushua – good luck in your ongoing recovery!