Dermatology patients need better access to psychological therapies – but GPs can help
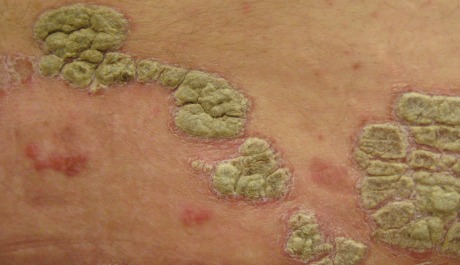
In an era of social media, people can be cruel when commenting on the appearance of those with skin conditions. Often patients are reluctant to share the emotional impact of their condition for fear of being seen as vain or because of a sense of hopelessness as to what their GP can do to help.
Alarmingly The All Party Parliamentary Group on Skin (APPGS) reported in 2013 that the provision of psychological support to dermatology patients has not improved since its last investigation in 2003. Common psychological difficulties described by patients include increased levels of anxiety and depression, concerns with body image, lowered levels of self-esteem and worry about social interactions. There have also been cases of suicide associated with depression triggered by psychological distress associated with a range of skin conditions.
GPs may find that providing patients with skin conditions space to disclose their feelings can be a sufficient intervention
The need for access to psychological interventions has been stated in a number of recent NICE guidelines. For example, the effect of psoriasis on psychological and social wellbeing should be assessed as part of routine management in general practice, and referral for psychological support should be provided where necessary – but how often does this actually happen?
We recently conducted a brief survey via The Primary Care Dermatology Society focussing on the support available for two common skin conditions: rosacea and psoriasis. The survey, completed by 48 GPs with a specific interest in dermatology, indicated that over 75% of respondents saw a clear psychological impact in their patients with both rosacea and psoriasis, yet fewer than 15% reported being able to refer their patients to a psychologist or other psychological service because of lack of provision for psychological support for skin conditions. Meanwhile, 85% commented that more help for patients with dermatological problems should be made available.
Although we all need to be lobbying for easier access to psychological support for this group of patients, GPs may also find that providing patients with skin conditions space to disclose their feelings can be a sufficient intervention.
GPs could consider routinely asking patients about their subjective perception of the severity of their skin condition. Simple 1-10 subjective severity scales can be easily woven into brief consultations to see if you need to consider a more detailed assessment. You can also routinely use brief questionnaires to assess psychosocial distress and impact on quality of life when a patient appears distressed or scores highly on using a subjective severity scale. Measures such as the GAD7, PHQ9, and DLQI can be particularly useful.
You could also signpost patients towards or provide patients with advice on self-help resources. Habit reversal has been shown to be effective in managing scratching and there are resources for self-help for managing itch associated with atopic conditions. Recently the British Association of Dermatologists launched a website containing several self-help resources and guidance for patients on assessing the impact of their skin condition.
Acknowledgments: The survey mentioned in this article was funded by a grant from The University of Sheffield and by Galderma UK Ltd.
Dr Andrew Thompson, is a reader in clinical psychology at the University of Sheffield, works as a Clinical Psychologist, and is psychological adviser to the all party parliamentary group on skin.
Dr Abigail Millings is a lecturer in psychology at the University of Sheffield.
Dr Marta Krasuska is a research associate in psychology at the University of Sheffield.
Dr Anastasia Lavda is a lecturer in clinical psychology at the University of Sheffield and a clinical psychologist.
Have you got a view you want to share with Pulse?
We’re always open to first-hand pieces and opinions from GPs.
Email your piece for consideration to be published on our site.
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.













