Even the DDRB admits this GP pay review may not add up

The 2014 pay uplift announcement will be the last I’ll cover as editor of Pulse, but after seven years here I’ve become all too familiar with the drill.
A terse press release from the Department of Health, setting out the bare bones of the deal. The considered report of the Review Body on Doctors’ and Dentists’ Remuneration (still universally known, to the confusion of acronym pedants everywhere, as the DDRB). An angry response from the GPC. And then scepticism from medical accountants, who invariably end up pointing out that once expenses are properly taken into account, GPs won’t end up taking home nearly as much as the health secretary thinks they will.
A familiar ritual then, but a significant one nonetheless as practices gird their loins for the financial year ahead. And while the outcome of this year’s pay review may seem like the same old story – a small promised pay rise which will almost certainly fail to materialise – the details of the DDRB report offer two curious twists.
Staff expenses
First, staff costs. The top line of this morning’s announcement immediately caused confusion with its assertion that a practice funding uplift of just 0.28% would result in a 1% net pay rise for GPs. Such an outcome could only be accounted for by falling expenses – and if you look at the number-crunching in the DDRB report, that indeed seems to be the case. According to the DDRB average GP staff costs have fallen 1.4%, and because of their relative importance or weighting this more than cancels out a 2.7% rise in other practice expenses.
Surprised? As one reader put it succinctly: ‘There’s been a drop in staff costs? In which universe?’ Well, actually the estimate is based on something called the Annual Survey of Hours and Earnings, compiled by the Office for National Statistics, and the DDRB robustly defends its use.
The BMA told us that it supported our continued use of the Annual Survey of Hours and Earnings (ASHE) to represent movement in staff costs. The Department of Health’s evidence for this year asked us to consider what allowance should be made for practice staff pay in line with other sectors of the NHS workforce, and the Scottish Government thought ASHE to be the best official source of information. We discuss the issue of the appropriate coefficient to represent staff costs in Chapter 3: we conclude that ASHE continues to be the most appropriate indicator.
Yet it gets more complicated. The Department of Health this year followed the DDRB’s recommendation, but last year it didn’t. One reason it didn’t is that it believed the DDRB’s estimate of GPs’ staff costs was flawed – even though it was calculated using exactly the same ASHE estimates.
The DDRB report goes on to say:
We have already noted our disappointment last year with the Health Departments’ decisions not to accept our recommendation for GMPs, especially as the reason for the rejection was apparently based on our use of the ASHE general medical practice activities 2012 figure of 3.4%, which might have appeared to be higher than one might have expected. The equivalent ASHE figure for 2013 is -1.4%, suggesting that taken over a longer period, it does not appear to be outside the range of what one might expect to be reasonable.
So what should be done about it? Well, the DDRB’s suggestion is somewhat radical.
We are not proposing to make a compensating adjustment to our recommendations, but note that the Health Departments are able to revisit last year’s decision on the uplift in combination with this year’s recommendation to account for the longer-term trajectory of ASHE, should they consider it appropriate.
That, it seems fair to say, appears to have fallen on deaf ears at Richmond House.
A flawed formula
Where things get even more interesting, though, is in the DDRB’s frank assessment of the accuracy of its own uplift calculations.
The GPC has long argued that the DDRB’s number-crunching fails to take proper account of GPs’ expenses and consistently results in much lower-than-intended net pay uplifts. And this year, it seems, the DDRB has done the maths and agrees.
The following table, from page 42 of the DDRB report, provides a fairly damning five column summary of the current funding crisis in general practice.
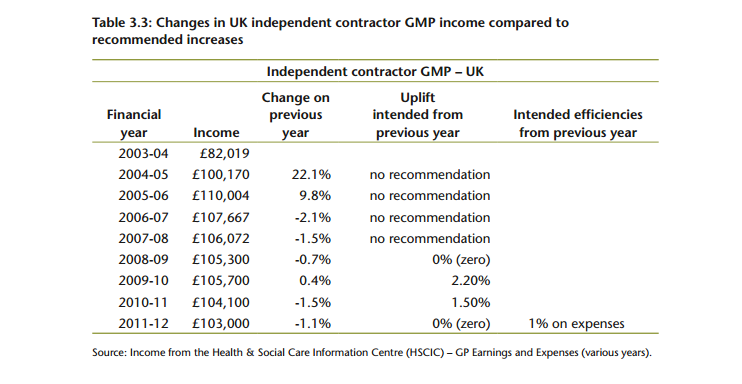
Of course, the pattern is further complicated in years when the Department of Health chooses not to follow the DDRB’s recommendations. But in the years when it does, there seems to be a pretty obvious trend. As the report puts it, with commendable understatement: ‘The data shows that the movement in average income appears not to correspond with the intended increases behind our recommendations.’
Why is that? Well, the DDRB offers several pages of speculation – the formula may not take proper account of efficiencies at practices, private work could be a complicating factor, correction factor payments and QOF achievement could skew things, and so on.
But whatever the reason, the conclusion is clear, and the DDRB doesn’t pull its punches. ‘Having taken into account all of the above, we have serious reservations about continuing to make recommendations using the existing flawed formula-based approach,’ it says.
It then sets out a long list of additional data it requires to try and make that formula more robust, and adds:
We ask the parties to report back to us next year on what progress they have made in taking forward the issues we have highlighted above. In the absence of such information, we were minded to focus on recommendations on pay, which is of course the core part of our remit. However, when we explored this possibility with the parties during oral evidence, the clear and over-riding message that we took back was that despite serious and well-understood shortcomings with the formula-based approach, the parties found our recommendations that included the various elements of expenses to be helpful. We are therefore willing to use the existing formula-based approach for 2014-15 for both [GPs] and [dentists[. However, we attach such importance to the provision of better data that we are recommending that significant progress is delivered to us in time for our next review. Without such data, we have strong reservations about the use of a formula-based approach to deliver an uplift in line with our intentions.
So there, in carefully worded civil servant-speak, you have it. The DDRB has made a recommendation, but has no confidence that the uplift it has recommended will deliver the 1% uplift it would like and the Government has promised. GPs can hardly be blamed for sharing those doubts.
Steve Nowottny is the editor of Pulse. You can follow him on Twitter @stevenowottny.
Have you got a view you want to share with Pulse?
We’re always open to first-hand pieces and opinions from GPs.
Email your piece for consideration to be published on our site.













