The case
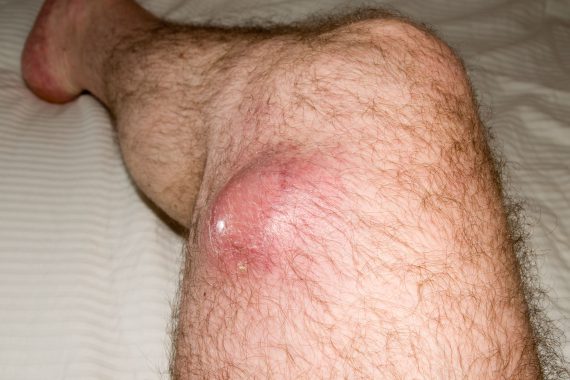
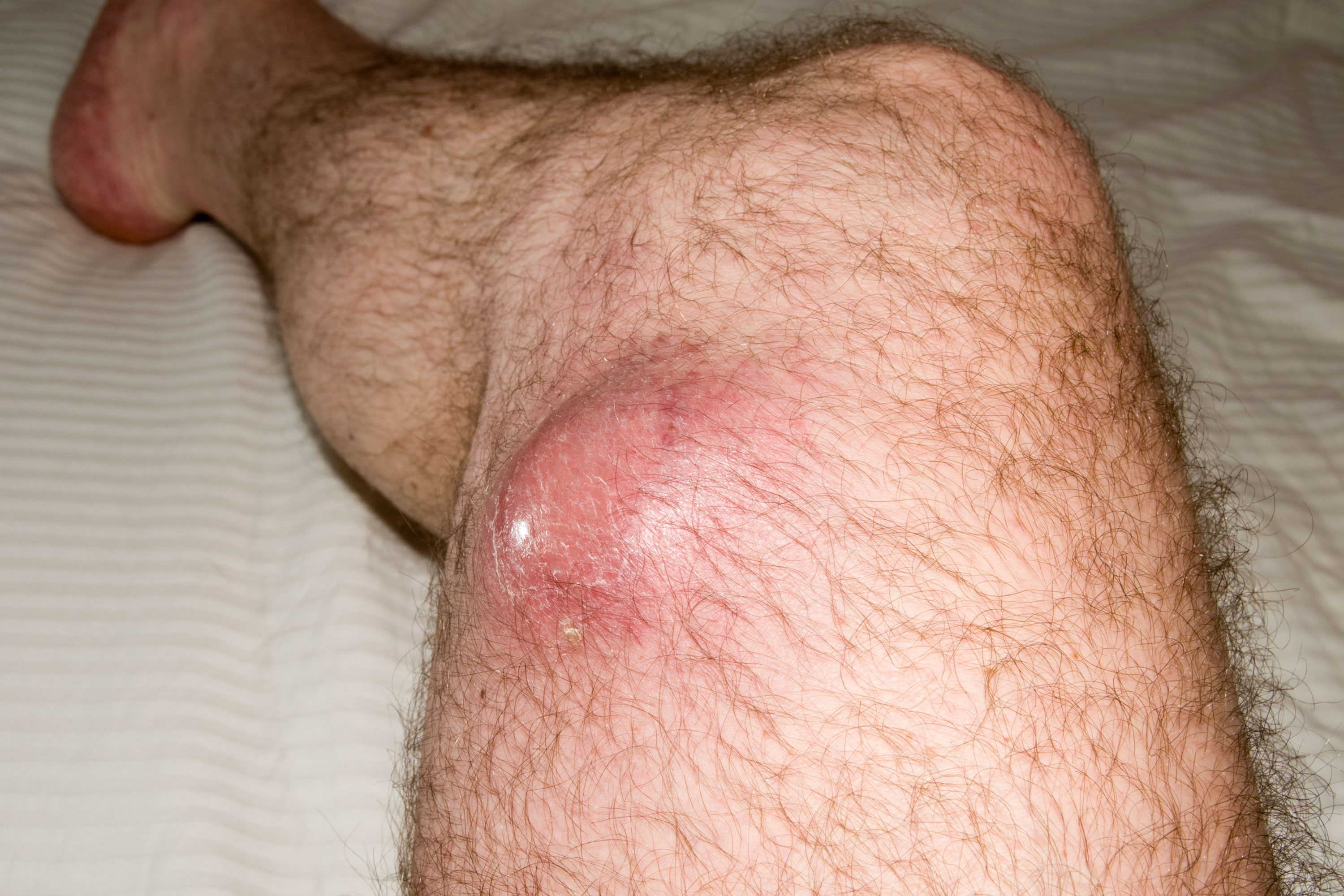
A 50-year-old man presents to his GP with a four-month history of a painless enlarging swelling on his thigh. It has now started to affect his walking. Examination reveals a swollen left thigh, with a mass, fixed to underlying muscle. The GP suspects a soft-tissue sarcoma (STS) and urgently refers him to an orthopaedic surgeon. An MRI scan demonstrates a suspicious mass, and the recommendation is to refer to the local sarcoma unit.
The problem
STSs are a heterogeneous group of rare tumours arising from the mesenchymal tissue, accounting for approximately 1% of all adult cancers. Approximately 3,000 new cases are diagnosed in the UK each year.1 It can occur at any anatomical site, with more than 100 different histological subtypes, and has a predilection for deep locations in the extremities and limb girdle.2 These tumours are challenging to diagnose early-on, due to a combination of histological heterogeneity, variable anatomical primary site and rare incidence. However, the majority of soft-tissue tumours are benign, outnumbering STS by a ratio of 100:1.3 The survival of patients with STS is dependent upon adequate and timely resection and, in selected high-risk cases, neoadjuvant or adjuvant radiotherapy. Benign lesions are managed less aggressively.
Features
STS most commonly arises in the lower extremities and girdle (40%), upper extremities and girdle (20%), trunk (10%), retroperitoneum and viscera (20%), and head and neck (10%) sites. Some histological subtypes have a predilection for certain anatomical sites. Tumours can grow at different rates but tend to follow tissue planes, limited by bone or fascia, and are usually bound by a capsule. They commonly present as a painless, enlarging mass. Some tumours can present when very large, usually the thigh and retroperitoneal sites, and occasionally show compressive symptoms. Patients do not usually present with constitutional symptoms such as weight loss or fever.
Most patients will present with localised disease (10%), although the risk of metastatic disease increases with several factors, including primary tumour size, depth, if it is of a high grade, and histological subtype, such as Ewing’s sarcoma. Metastatic disease predominantly affects the lung in 80% of cases that have metastasised, although the liver, bone and brain can also be affected. Regional nodes are rarely involved, and are only seen with a few histological subtypes.
Most common histological subtypes seen in adults
- Undifferentiated pleomorphic sarcoma (UPS)
- Liposarcoma
- Leiomyosarcoma
- Synovial sarcoma
- Malignant peripheral nerve sheath tumor (MPNST)
- Rhabdomyosarcoma
- Fibrosarcoma
- Extraskeletal Ewing’s sarcoma
- Angiosarcoma
Diagnosis
Features that should prompt consideration of an urgent two-week rule referral of a soft-tissue lesion include:4
- A soft-tissue mass more than 5cm, the size of a golf ball size or larger
- A painful lump
- A lump that is increasing in size
- A lump of any size that is deep to the muscle fascia, fixed or immobile. This can be assessed clinically, as organising investigations can take time.
- A recurrence after previous excision
If STS is suspected, then an early referral to a sarcoma centre or designated diagnostic centre is essential, as per NICE guidance and their local guidelines. Preliminary investigations include ultrasound or cross sectional imaging, to differentiate between benign and malignant lesions (dependent on the experience of a radiologist), assist surgical planning, and – if STS is confirmed – to exclude metastases. The histological diagnosis is made using a core needle biopsy, either in a sarcoma unit or by a designated centre. Fine needle aspirations are not recommended in the initial evaluation, as they may not allow histological subtype to be characterised.
Management
Early referral to a sarcoma centre is essential where patients are managed within a multidisciplinary team.5 The principles for treating local disease are to improve survival, reduce local recurrence, maximise function and reduce morbidity. Wide local excision of the primary tumour without cutting into tumour tissue is essential, to reduce the risk of local recurrence. Unplanned tumour violation, more commonly referred to as the ‘whoops procedure’, or a resection with a gross or microscopic residual tumour and positive margin, is associated with a higher risk of local recurrence.6 Combining limb-sparing surgery with radiotherapy has demonstrated better local control than surgery alone for selected STS cases, including large primary, high grade, deep seated tumours over 5cm.
Patients with metastatic disease can be managed using observation, or palliative therapies, such as systemic chemotherapy, or radiotherapy. Selected patients with low volume metastases may benefit from more aggressive local treatment, like surgery, radiotherapy or radiofrequency ablation.
The insidious and variable presentation, heterogeneity of histological subtypes, and wide variety of anatomical primary sites, may explain the lack of experience in diagnosing and treating sarcomas outside specialist centres. Since benign soft-tissue tumours outnumber STS, primary care physicians are unlikely to see many STS during their career. A delayed diagnosis can have a negative impact on the possibility of an uncomplicated resection with clear surgical margins, and potentially increases the risk of developing metastatic disease.7 There is a need to improve the diagnostic pathway for STS through increasing education and improving collaboration between specialist sarcoma centres, referring institutions and GPs.
Dr Shane Zaidi is a consultant clinical oncologist at the Royal Marsden NHS Foundation Trust
Mr Myles Smith is a consultant surgical oncologist at the Royal Marsden NHS Foundation Trust
Dr Christina Messiou is a consultant radiologist at the Royal Marsden NHS Foundation Trust
Dr Khin Thway is a consultant histopathologist at the Royal Marsden NHS Foundation Trust
Dr Robin Jones is a consultant medical oncologist at the Royal Marsden NHS Foundation Trust
References
1. Cancer Research UK. Soft-tissue sarcoma statistics. Available at: http://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/soft-tissue-sarcoma#heading-Zero
2. Fletcher CDM, Bridge JA, Hogendoorn PCW, Mertens F. World Health Organization Classification of tumours of soft tissue and bone. IARC Press, 2013.
3. Canter RJ, Smith CA, Martinez SR et al. Extremity soft tissue tumor surgery by surgical specialty: a comparison of case volume among oncology and non-oncology-designated surgeons. J Surg Oncol, 2013;108:142-7.
4. Sinha S, Peach AH. Diagnosis and management of soft tissue sarcoma. BMJ, 2010;341:c7170.
5.NICE Guidance on Cancer Services: Improving Outcomes for People with Sarcoma. National Collaborating Centre for Cancer, 2006.
6.Qureshi YA, Huddy JR, Miller JD et al. Unplanned excision of soft tissue sarcoma results in increased rates of local recurrence despite full further oncological treatment. Ann Surg Oncol, 2012;19(3):871-7.