Working life: The osteopath GP
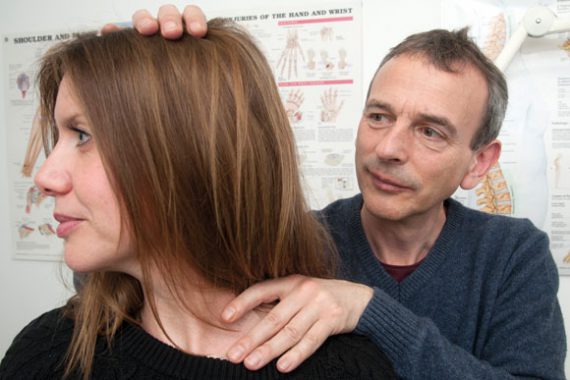
Profile – Dr Nick Mann
Roles
Qualified as Bachelor of Medicine, Bachelor of Surgery in 1990, MRCGP in 1995 and osteopath in 2011. Teaches paediatrics, obstetrics and gynaecology, and musculoskeletal medicine in primary care
Hours worked per week
Part time after children were born, but now 40 hours per week. Salaried for 29 hours per week
Monday
Today I visit frail 92-year-old Mrs H, who has ‘put her back out’. Functional release relieves her pain and restores her independence. I find osteopathy treats these conditions more enduringly than physiotherapy, and is safer than a chronic NSAID or opiate prescription.
It was my own experiences as a patient that led me to osteopathy. A neck injury in 1990 deteriorated into disc problems, radiographic spinal stenosis and complex regional pain syndrome. After a year in which I was unable to work, osteopathy brought me to recovery and allowed me to avoid spinal surgery.
These days, I’m a salaried GP in a large NHS practice in Hackney, east London, and teach community paediatrics and obstetrics and gynaecology to fourth-year medical students. I also run the practice’s locality joint injection service.
Training as an osteopath has allowed me to treat musculoskeletal problems directly. Typically, 50-60% of my workload is musculoskeletal. I mostly use high-velocity low-amplitude thrusts (HVLAT), or osteopathic manipulation, but this method is not always appropriate, such as for the elderly.
Tuesday
I’m seeing a 30-year-old patient who had been signed off his managerial position with spinal pain which had put him in a wheelchair. He had thorough investigations, neurosurgery referral, physio and pain clinic input, without improvement. After months of osteopathy treatment and rehab, he has returned to work – free of his wheelchair.
Structural diagnosis enhances my understanding of musculoskeletal pain, radicular and non-radicular symptoms, and evolving serious pathology. This means I can target investigations, referrals and treatment accurately from primary care, and can prevent a volume of referrals as well as repeat presentations and chronic opioid usage.
Wednesday
Chest pain is a common reason for presentation to both GPs and A&E. Individuals with musculoskeletal chest pain often undergo unnecessary investigations for other serious diagnoses.
A 50-year-old woman had seven weeks of left-sided chest pain, affecting her breathing. She visited A&E twice, having bloods, chest X-ray, stress echocardiography and pulmonary angiogram before demanding I refer her for an MRI scan. It’s usually possible to reach a positive diagnosis of musculoskeletal chest pain and treat it directly, and this was the case here – the patient’s pain and fears were relieved by a single HVLAT.
Thursday
I see a businessman in his 30s who became depressed after knee pain stopped him playing sport. Despite adherence to physio regimens and investigations by private orthopaedic surgeons, his pain was worse. I saw him four weeks ago and he was dismissive when I found a locked segment in his lumbar spine. Yet when I review him now, he is immensely relieved. Such happy endings reinforce my passion for what I do.
Friday
Debilitating low back pain (LBP) is the last thing a mother needs after childbirth. Even years on, I’m finding a large cohort of patients with symphysis pubis dysfunction, radiating LBP and coccyx, hip and knee pains, caused by a demonstrable twist in pelvic alignment, likely from birthing. Today, I see a new mum, who was told it was not surprising she had pain as she was very overweight. She was needing stronger analgesia than NSAIDs, but worried about taking co-codamol while breastfeeding. But realigning her pelvis took two HVLATs and just 10 minutes – curing her without drugs.
Saturday
Beyond the traditional working week, I’m also a tutor, mentor and trustee at the London College of Osteopathic Medicine. It’s disappointing there’s no formal support for GP osteopaths in the NHS as, with knowledge of our patients’ comorbidities and medications, it’s particularly suited to general practice. But I’d recommend this training to any doctor.
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.










