Crisis point: GP partner shortage hits practices


Murmurings of an impending GP recruitment crisis have been circulating for a while. Now, according to the GPC, that crisis has finally arrived.
An internal briefing paper – seen by Pulse – says the effects could be ‘catastrophic’, with general practice suffering permanent damage.
A Pulse investigation shows that one in 10 partnership vacancies goes unfilled for more a year, and a quarter are vacant for more than six months.
This is putting immense strain on to practices, with workload mounting and GPs struggling to meet patient demand.
Even practices in prosperous parts of the country are finding it hard, with some resorting to offering £20,000 ‘golden hellos’ to attract partners.
The situation seems to be rapidly deteriorating, and there is little sign of any reprieve.
‘The time has come to declare that the workforce gaps in general practice have reached crisis point’
GPC briefing paper on the recruitment crisis
Toxic cocktail
Pulse has learned that education chiefs have stepped in with thousands of pounds of emergency funding to support practices in one area that is down to one GP per 8,000 patients. But this is little more than a temporary fix for a toxic cocktail of problems in general practice.
The GPC briefing paper lists rock-bottom morale and rising workload as major reasons for many GPs rejecting partnerships and choosing instead a better work-life balance as a sessional GP.
‘The time has come to declare that the workforce gaps in general practice have reached crisis point,’ it declares.
‘There is an unwelcome lack of certainty in responses to advertisements for partnerships and sessional roles. Overall, the picture would suggest that practices around the UK are unable to recruit and replace GPs.’
The GPC’s conclusion pulls no punches: ‘The effects on patients and profession alike will be catastrophic.
‘Without drastic steps of action taken now, UK general practice will suffer permanent damage. The truth is that corporate bodies will want to fill the gap if practices start to fail.’
‘If we cannot recruit anyone here, how is the rest of the country doing?’
Dr Andy Ward, a GP in the seaside town of Weymouth, Dorset, has personal experience of the difficulties described in the GPC paper.
He says: ‘One of our partners left two years ago. We advertised locally and had no applicants. We then headhunted somebody, who turned out not to want to stay. We advertised nationally back in January, and had no applicants at all.
‘We are not in a part of the world where we have had problems before. We are a small, friendly, high-earning practice. Morale here is good and it is a great place to live. If we cannot recruit anyone here, how is the rest of the country doing?’
At the other end of the country, practices are experiencing similar problems. Dr Jane Lothian, medical secretary of Northumberland LMC, says: ‘My own small practice gave up trying to recruit doctors and ended up building around nurse practitioners. We were looking for a year and a half.’
She says the problem is getting worse in her area, and that practices are suffering badly: ‘In the south east of Northumberland, where the old coalfields are, it has been quite a problem and it is getting worse. Some practices in have up to three doctors’ worth of vacancies.’
Why does no one want to be a partner anymore?
• ‘Alarming’ increases in the levels of stress felt by GPs.
• Denigration of general practice by Government and in the national media.
• Younger doctors demanding more flexible career options and current training leaving GPs ‘woefully underprepared’ for life as an independent GP.
• Lack of control over work-life balance and underinvestment in general practice.
• Lack of support for returners and retainers.
Source: Recruitment of GPs: Time to take action for the future workforce, presented to the GPC April 2014
Few candidates
The problem is spreading. A recent survey of 270 practices across the south of England by Wessex LMC shows 70% had a vacancy to fill in the past year, of which almost one in three was unsuccessful.
Cleveland LMC found GPs receive an average of three applications for a partnership post; typically, one of these pulls out and one is unqualified, leaving a single potential candidate.
Pulse has learned that one practice in a ‘relatively leafy, affluent’ part of Doncaster, South Yorkshire, has had to offer partners a £20,000 ‘golden hello’ to join and stay at the practice.
Local LMC chair Dr Dean Eggit says such measures are not surprising. He has found that a number of practices in his area have long-term recruitment and retention problems.
He says: ‘My last understanding of the “golden hello” was that it was used in the early 1990s, when there was exactly the problem that we are starting to get to now. Patient demands and expectations cannot be met, so there are long working hours et cetera. There are not enough doctors nationally.’
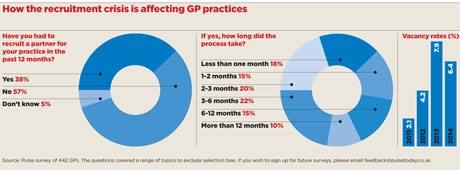
A Pulse survey of 442 GPs across the UK confirms that many practices have to cope with vacant posts for long periods. More than a third (38%) have had to recruit a partner in the past 12 months, and the process lasted more than six months for 25% of them and in excess of a year for 10% of respondents.
‘‘Three of us are going in two years. The effects are insidious’
Dr Eamonn Jessup, chair of North Wales LMC and a GP in Prestatyn
In North Wales there have been longstanding issues for GP recruitment and retention, but Dr Eamonn Jessup, chair of North Wales LMC and a GP in Prestatyn, says his practice has spent ‘thousands’ on advertising posts in the past 12 months, as they are four GPs short of the nine required, and have had no suitable candidates.
‘We have not had a single applicant,’ Dr Jessup says. ‘Three of us are going in two years. The effects are insidious: the numbers of referrals we are sending off is increasing because we are not now able to review the patients. Prescribing is going up.’
This has led the practice to consider drastic measures: ‘The next step for us is to appeal to those GPs losing MPIG in England to come and join us. It’s business. The fact is, we are desperate, and dare I say it, it is dog eat dog.’
Meanwhile, locum agencies and chambers are booming. Dr Richard Fieldhouse, clinical director of the Pallant Medical locum chamber, based across the south of England, and chief executive of the National Association for Sessional GPs (see Day in the Life, page 104), says that around 50% of his chamber’s new members are ex-partners who are joining despite often experiencing a pay cut.
He says: ‘They feel that the chambers is a more supportive environment than a partnership; they can just focus on quality of care.’
Overwhelmed
Conversely the recruitment crisis means the chambers are overwhelmed with work. Dr Fieldhouse says: ‘In just one CCG area, we have had 12,500 requests for sessions to be filled and we have only been able to fill 9,000 of them.
‘The reason for this is that practices cannot recruit partners or salaried GPs, and doctors are going off work stressed.’
It was only three years ago that there was another workforce crisis – but that involved salaried GPs being unable to obtain partnership posts, with the RCGP posing the question at its annual conference: ‘Is the profession doing its newly qualified colleagues a disservice with the lack of partnerships available?’
Now, for perhaps the first time, young doctors do not see partnerships as being an attractive career path and are opting for sessional roles.
Dr Lothian says this is leading to practices in Northumberland thinking about offering innovative ‘joint posts’ with secondary care to attract younger doctors to general practice. She says: ‘We’re setting up joint posts so young doctors can rotate through primary and secondary care after they have done their MRCGP. We see they still want variety. Some practices are looking at offering flexible posts – terms out of the contract, that sort of thing.’
Experienced GPs leaving the country or retiring is also exacerbating the problem. GPC deputy chair Dr Richard Vautrey says: ‘There are large numbers of older GPs who are retiring early. They are struggling to cope with the workload and constant bureaucratic annual change in what is asked of them, and so with the punitive pension changes, they have decided that enough is enough.’
Those causes of the current crisis are not going to go away anytime soon, but there are signs NHS bosses recognise the situation is unsustainable.
The RCGP is calling for the NHS to make it much easier for GPs to return to practice. Currently, GPs must apply to their deaneries, who then identify a practice where they can be mentored before they go back on the performers list. RCGP chair Dr Maureen Baker has made it a priority to remove these barriers. These ideas are being looked at by the Department of Health.
Fire-fighting
In Essex, Health Education England has offered practices a share of a £400,000 firefighting fund, after Pulse revealed in January that problems with recruiting had left one area in the region – Frinton-on-Sea – with one GP to 8,000 patients. The money is only a temporary solution designed to hire locums and increase practice nurse numbers, but GP leaders have welcomed the intervention.
Essex LMCs chief executive Dr Brian Balmer says it is ‘early days’ but hopes the additional funding will alleviate the immediate problems: ‘We are wanting to get on with it quickly, and it will be support for sessional doctors and more apprenticeships.’
And in a more unusual step, a housing developer in Carlisle, Cumbria, in a joint scheme with the local authority, has offered GPs a discount on home-buying in a bid to attract them to the areas in which it is currently building.
In an offer open until March next year, Story Homes is offering a £1,000 discount for every £50,000 spent by GPs on its developments in four areas of the town.
‘The number of jobs coming up is reducing, simply because nobody has money to buy doctors anymore.’
Skill-mix
Pulse’s survey shows that although vacancy rates remain high, they are slightly lower than those shown by a similar Pulse survey last year. Overall, there was a 6.4% vacancy rate, compared with last year’s figure of 7.9%, although this still represents a steep rise on vacancy rates of 4.2% and 2.1% from similar surveys in 2012 and 2011, respectively.
Dr Eggit says this drop in vacancies is a sign plummeting incomes are starting to limit the number of partnerships practices can offer, and that some are having to look for other solutions.
He says: ‘The number of jobs coming up is reducing, simply because nobody has money to buy doctors anymore. In my own practice, we would love to be able to recruit but the money is not in the pot.’
Dr Vautrey concurs: ‘Practices are experiencing big funding cuts now, and if they are PMS they face even bigger cuts just around the corner, so they are having to seriously look at whether they can afford to replace GPs who are leaving.
‘Some also have reluctantly accepted that they can’t recruit to vacancies and therefore had to look for other alternatives in terms of skill-mix.’
The Government has made a great play of its plans to boost GP numbers in the future, although its target of having 3,250 trainees entering general practice has recently been delayed by a year until 2016, which offers little help to practices wanting to recruit now. The recruitment problems in general practice look set to get much worse before they get better.
Ten steps to successfully recruit a partner
Read Dr Simon Poole’s quick guide on how to find a new GP
Pulse July survey
Take our July 2025 survey to potentially win £1.000 worth of tokens












