
hms partner ship 3×2
‘I was finding it increasingly overwhelming, becoming more and more demoralised, short tempered and tired. I took time off ill, and felt I could no longer do medicine,’ recalls Dr Tina Sumner. ‘As I recovered, I asked myself what I liked about the job and came to the conclusion I wanted to be a clinician, to see patients. I made the decision to resign from my partnership.’ The Hampshire GP is now set to take up a salaried role.
And she is not alone. GP partners are increasingly concluding that life may be better as a salaried employee, to escape from the pressures of partnership.
A Pulse survey has revealed that more than half of partners said that they would now consider becoming salaried if offered the right deal, while only one in five GPs feels the current partnership model will exist in 10 years’ time.
Pulse has learned of scores of practices where all the partners are planning to become fully salaried.
In England, NHS England’s Five Year Forward View is quietly driving a move among practices to hand back their contracts, with GPs willing to work in salaried roles for foundation trusts, GP federations or under the ‘new models of care’.
And in Scotland and Wales, health boards are increasingly taking over contracts – and practice staff – when retiring partners cannot be replaced.
Unthinkable
This has crept up on the profession. As recently as 2009, giving up partnerships in favour of a salaried career would have been unthinkable. That year, the BMA called for the Government to restore central control of GP recruitment in a desperate attempt to increase the number of partnership roles available to young GPs, who were being forced into salaried roles against their wishes.
How times have changed. Decreased funding, increased demand, the advent of CQC inspections and widespread problems with GP recruitment, among many other reasons, have significantly reduced the appeal of partnerships.
Official figures show that in September 2009, 69% of all GPs in England were partners while 20.5% were salaried; in September 2015, this had changed to 55% and 24%.
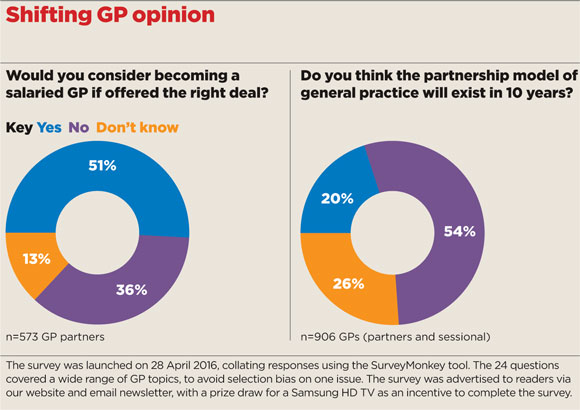
shifting gp opinion box 580x410px
Leeds GP Dr Sarah Lawton says she gave up partnership two years ago and it has been ‘absolutely wonderful’. She adds: ‘I enjoy my work, I go in to see patients. When I was a partner, I was always late, because I was at a meeting or signing something… It is so much less stressful, and everyone says I am smiling more.’
Bristol GP Dr Shaba Nabi is another to make the switch. Last month, she announced in her Pulse column she was resigning from a partnership role ‘that 10 years ago was being pursued by hundreds of applicants and I felt so proud to achieve’.
Dr Nabi says she made her decision after taking a burnout survey, but the money differential was also a factor.
She adds: ‘Although there is still a gap in pay between partnership and salaried roles, it is definitely decreasing.’
Pulse’s survey of more than 500 GP partners in May showed a growing number are thinking along these lines.
It revealed more than half of partners in the UK (51%) would consider going salaried if presented with the right deal. Only 36% said they would not.
The survey also revealed dwindling faith in the future of the partnership model, with 54% of respondents saying they do not expect it to survive 10 years, and only 20% saying they do. This compares with 50% and 23% in October.
Meanwhile, a BMA survey last year showed that almost two-thirds of sessional GPs as a whole do not envisage seeking a partnership in the future.
This shift is being borne out on a greater scale. Pulse has learned there are several areas where whole practices are asking to have their contracts taken over, with all the partners becoming employees of larger organisations.
In Gosport, Hampshire, the local community trust is one of many organisations testing the ‘new models of care’ outlined in the Five Year Forward View – designed to implement plans for single organisations to provide both primary and secondary care.
Six of the 11 GP practices in the town have reached out to the Southern Health NHS Foundation Trust to take over their practices and allow the GPs to become employees of the trust.
Dr Stuart Morgan, a senior partner at the Brune Practice in the town, wrote to patients explaining partners had been ‘overwhelmed by the perfect storm’ of a reduction in GP funding, soaring workload and the ‘unprecedented’ recruitment and retention crisis. As a result, the partners were ‘working hard to create a solution: a partnership with Southern Health that provides a continuation for you, and for the team at Brune’.
GP lead for the South Hampshire new model of care Dr Donal Collins tells Pulse the practices were desperate. ‘They would get half a partner, and it would be like a breath of fresh air, but then it would dip again. When you are in a bad place, the ability to create change is easier,’ he says.
Meanwhile, the Royal Wolverhampton NHS Trust took on the contracts of three practices in June as part of a pilot to integrate primary and secondary care and cut emergency admissions.
But Dr Julian Parkes, a GP who has become salaried under the trust, says making life more tolerable for GPs was also a factor. He says: ‘We want to see a better service for patients and less stress for GPs. We have lost the grief of being a small business and issues with staff .’
A similar model of care in Somerset could soon hold as many as 10 GP practice contracts, employing all former partners. Three practices handed their contracts to the trust in April and another six or seven are in talks to do so.
Hassle
In Hull, two practices approached the Yorkshire Health Partners GP federation to take over their contracts, which they did late last year. Dr Laurent Bare, a director at the federation, and a GP partner in East Yorkshire, says although partnership is a ‘fantastic’ model for practices, it is losing its appeal for GPs.
He says: ‘A lot of GPs, especially young ones, will think “do I have to become a partner when I can do nine to five and not have the hassle of running a business?”.’
In the devolved nations, health boards taking over contracts of practices in distress is already the default option. A BBC investigation last year found health boards had taken over 42 GP practices that could not recruit in Scotland.
In Wales, salaried models are also being driven by recruitment struggles, with health boards taking over 10 contracts from practices. Former health minister Professor Mark Drakeford told Pulse earlier this year the Government was supportive of ‘people who want to take experimental steps in that direction’.
Those staying in partnerships are also looking to offload premises commitments. Property development company Assura recently told Pulse it had increased its portfolio by more than a fifth within a year, with younger GPs increasingly unwilling to buy into premises.
But the partnership model is not on its last legs just yet.
The GPC remains resolutely in favour of it. Its blueprint for the profession – the Urgent Prescription for General Practice – last year recommended commissioners take advantage of ‘inherent flexibilities’ of the independent contractor model when developing new models.
While at the Special LMC Conference convened in January, LMCs voted against a motion to explore ditching the independent contractor status.
Last year, Scottish GPC chair Dr Alan McDevitt said contract negotiations were looking at a model ‘as close to salaried as possible’. But the plans were watered down after a survey found 85% of GPs wanted to retain independent contractor status.
Dr McDevitt says: ‘We fully intend to strengthen the independent contractor model, with a clearer role for GPs and a clearer payment system to be an “expert medical generalist” with practices and their registered list continuing.
‘Salaried options will remain and are the current default if a practice becomes unsustainable but we believe the future is a strong, modern independent contractor GP model leading a broader primary health care team to better outcomes for patients.’
But a picture is emerging of a GP workforce that supports the independent contractor status in principle – but not necessarily in practice.
What’s happening across the country
Wolverhampton
Pilot project where former partners at three GP practices are being employed by the Royal Wolverhampton NHS Hospitals Trust. Dr Julian Parkes, who has become salaried at the trust, says it will be ‘a better service for patients with less stress for GPs’.
Gosport
Six practices will become salaried under the auspices of the local trust, testing the ‘new models of care’ outlined in NHS England’s Five Year Forward View.
South Somerset
New vanguard may hold 10 practice contacts, employing the current partners.
Hull
Local GP federation took over the running of two GP practices after an approach from partners, who have stayed on as salaried GPs.
East Yorkshire
NHS Humber NHS Foundation Trust took over 9,500-patient Market Weighton Group Practice on 1 April, after being approached by the partners after PMS cuts and recruitment problems.
Sheffield
A mental health trust and a GP provider company won an APMS contract in March to run five GP practices, covering 21,500 patients with a new salaried service.
Scotland
Health boards have taken over 42 practices due to problems recruiting. Scottish GPC chair Dr Alan McDevitt says under the new contract being negotiated for 2017, ‘salaried options remain and are the current default if a practice becomes unsustainable’.
Wales
Ten practices have been taken over by health boards while another eight are at risk, according to BMA data. Former health minister Professor Mark Drakeford told Pulse earlier this year the Government was supportive of ‘people who want to take experimental steps’ in the direction of a salaried model.
















