Will the NHS deliver 5,000 extra GPs by 2020?


forward view 2017 logo 580px
‘We are pulling out all the stops to try to double the growth rate in GPs,’ NHS England chief executive Simon Stevens said last year.
That statement confirmed the powers-that-be realise the current GP workforce situation is unsustainable, with vacancy rates continuing to soar, and practices often waiting 12 months to replace a GP.
As part of its GP Forward View, NHS England placed a big emphasis on increasing numbers to meet its target of 5,000 extra GPs by 2020, alongside 5,000 extra other practice staff.
Many of the pledges were a reiteration of those made the previous year, as part of NHS England’s so-called ’10-point plan’, including a ‘major recruitment campaign’, and ‘golden handshakes’ for GP trainees. It also announced they would recruit 500 GPs from overseas.
One year on from the GP Forward View – and two years on from the workforce plan – there have been some successes. But the problem for NHS England – and, more importantly, for GPs – is that far from expanding, the workforce appears to be contracting.
Indeed, official figures reveal that GP numbers decreased last year, despite all the measures implemented in 2015. And between September 2015 and December 2016, the number of whole-time-equivalent (WTE) GPs fell by 542 (1.6%).
GPC workforce lead Dr Krishna Kasaraneni says: ‘These figures underline just how far we are from meeting the Government’s target of recruiting and retaining more GPs as we near the first anniversary of the GP Forward View in England. Despite constant promises from ministers that the GP workforce would be increased by 5,000, the number of full-time GPs has fallen once again while the overall number has stagnated.’
The pledge to increase the GP workforce by 5,000 was made by health secretary Jeremy Hunt in the run-up to the 2015 general election, saying he aimed to attract the ‘best and brightest’ to the profession. Mr Hunt subsequently watered the pledge down to 5,000 ‘doctors in general practice’.
GPs were quick to point out that this would be nowhere near enough. The RCGP said 10,000 GPs were needed – and that was before factoring in plans for seven-day routine GP access.
Two years on from Mr Hunt’s announcement and there is little sign that even his modest target will be met. In the first 15 months of the drive, the WTE GP workforce fell by more than 500.
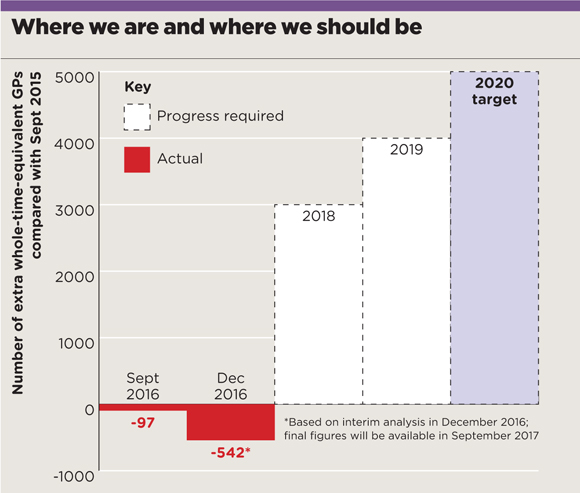
p10 april 2010 targets bar graph 580px
Retention
NHS England has announced an enhanced retention scheme to stem the flow, developed with the GPC and offering bursaries of up to £4,000 for those taking up the scheme. But so far, only 28 GPs have made use of this.
GPC sessionals subcommittee chair and Hull GP Dr Zoe Norris says although the scheme is ‘massively improved’ it is not enough for most people.
She says: ‘GPs of all ages are dropping partnerships to become sessional. So if the improved terms aren’t enough to counter the benefits of locuming, it won’t work.’
And the new figures do suggest this is a problem as the headcount of GPs is not falling quite as fast as that of WTEs and locum numbers are increasing.
None of the workforce measures can match the enormity of the problem
Dr Stephanie de Giorgio
In terms of attracting new GPs there have been successes: the GP training intake remains the biggest source of new GPs, and there was a 5% increase during the first round of recruitment for August 2017. NHS England and Health Education England failed yet again to meet their annual target of 3,250 graduates in GP training by 2016 but the 3,019 they managed was the highest number for at least seven years, before which recruitment rates were not published.
Equally, the ‘golden handshake’ scheme – offering £20,000 for trainees to work in areas that struggle to recruit GPs – has worked, with 105 of the 120 posts available last year filled. NHS England has offered 144 more this year.
Meanwhile, the ‘induction and refreshers scheme’ – designed to tempt back GPs on a career break or who have gone abroad – has brought back 76 GPs, with 300 more potentially in the pipeline. But Dr Stephanie de Giorgio, GPC member and a locum GP in Kent, says: ‘I don’t think it has attracted anyone who wasn’t already thinking of coming back.’
In fairness to NHS England, schemes can take time to bear fruit. Director of primary care Dr Arvind Madan says: ‘There is an inevitable time lag in some of the initiatives. For the I&R scheme, people will take time to get through the process. The right things are happening but they are not showing in the figures yet. In reality, around 4,000 of the 5,000 GPs will need to come through training, with NHS England finding the other 1,000.’
But as GPs point out, while such baby steps would have been welcome five years ago, the NHS now needs big strides. Dr de Giorgio says: ‘None of this addresses the main issue – that workload problems are the reason people are leaving. I don’t think any of the specific measures address that, and they would never have been able to match the enormity of the problem.’
As a result, the NHS has been forced to look abroad, despite the Government’s long-term aim of self-sufficiency. This year, 25 EU GPs have been appointed in Lincolnshire practices, with other areas such as Essex and Teeside following suit.
With Brexit now in progress, this may not be a sustainable source of workforce. But in the absence of a wider overhaul of general practice, looking abroad may be the only way to secure a short-term boost in GP numbers.
The start of GPexit?
The GPC found in 2015 that one-third of GPs was prepared to resign over the next five years, but until now there had been little sign GPs would follow through on that threat.
But these shocking new census figures show that the headcount of GPs in the health service in England fell by 402 between September 2015 and December 2016.
Admittedly this drop was lower than the 541 fall in the number of whole-time-equivalent GPs, suggesting that some GPs may have reduced their hours rather than left altogether.
But there also seems to be a growing trend for GPs to work as locums, with a 20% increase to 1,591 between September 2015 and December 2016.













