Ten top tips – distinguishing benign and malignant skin lesions
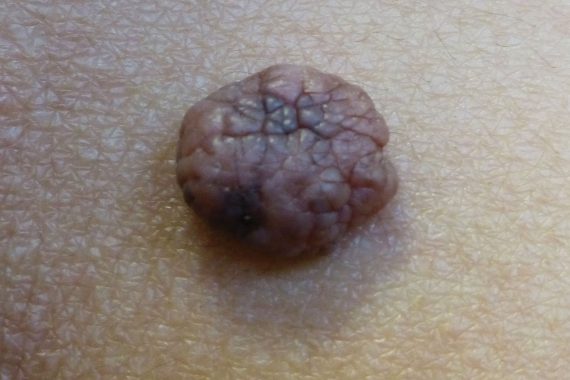
1 Soft, fleshy, compressible lesions are generally benign
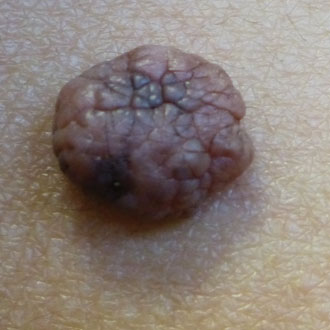
Skin cancers generally feel firm. Conversely, if a skin lesion is soft, fleshy and compressible, it is highly likely to be benign. The presence of hairs is a less reliable sign. These may often be found growing from a soft, fleshy, benign dermal naevus, such as the one pictured right. However, the presence of hairs growing from a firm lesion is not an infallibly reassuring sign, as hairs can be present in an early melanoma that has not yet destroyed the hair follicle.
2 Beware a history of rapid growth
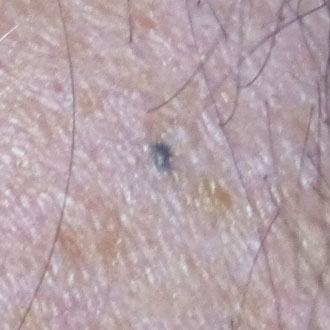
Beware a history of rapid growth in any skin lesion. Even if you think a lesion looks benign (for example, a keloid scar), if there is a history of rapid growth consider referral urgently. Genuine blue naevi are usually stable in size, so when a patient presents with this, always check the history to ensure this is the case. If a lesion looks like a blue naevus, but the patient gives a history of growth, this needs urgent referral.
3 Never ‘monitor’ a palpable lesion
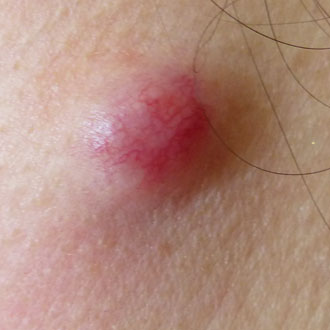
Never monitor an uncertain skin lesion that is already palpable. Thin melanomas can initially just spread laterally (superficial spreading melanoma), but once a melanoma has become clinically palpable it may have entered its aggressive vertical growth phase, which may make the prognosis far worse. The 2015 NICE melanoma guidelines state that monitoring may sometimes be appropriate for a lesion that is non-palpable and not atypical enough to need excision at first presentation, but this monitoring should be with photography and, ideally, this photography should be with a dermatoscope. If you see an uncertain skin lesion that is at all palpable, always refer urgently.
4 Multiple naevi can be typical or atypical
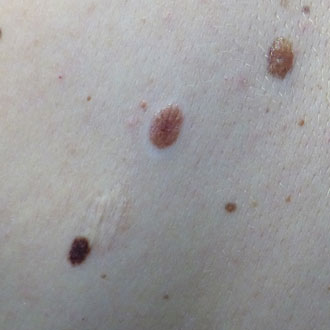
Multiple moles can be either ‘typical’ or ‘atypical’. Patients with more than 100 melanocytic naevi, or more than five atypical-looking naevi, are at higher risk of de novo melanoma. These can be very difficult to assess in primary care. If a patient has several typical-looking moles that all appear very similar, but there is an ‘ugly duckling’ among these, or they have multiple atypical moles, they need urgent referral. If a patient has multiple atypical-looking moles, they will generally be followed up by a dermatologist. In many parts of the UK, if a patient has multiple naevus syndrome, but all their moles are similar and typical looking, they may be discharged for self-monitoring.
5 Beware a single dark mole in a fair-skinned person
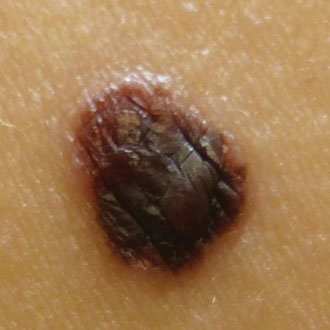
Moles in people with darker skin types are more likely to be dark in colour, and moles in people with lighter skin types are more likely to be lighter in colour. An individual person also tends to form moles that all have a similar ‘signature’ morphology. Melanoma of the skin also has a higher incidence in those with lighter skin types. So if a lighter-skinned patient presents with a single dark mole that is new or changing, even if the mole itself is less than 7mm and seems regular in outline and colour, consider urgent referral.
6 Beware a mole with three different colours
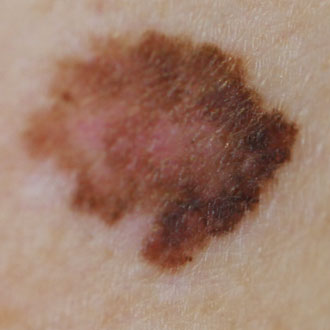
A mole containing three different colours (for example pink, brown and black) is always melanoma until proven otherwise.
7 Remember the importance of age
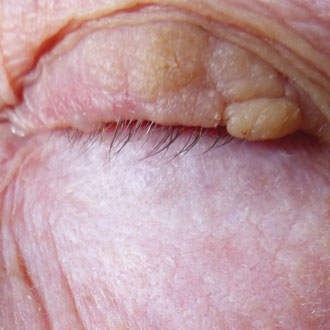
Over the age of 50 it is unusual to develop new benign naevi or moles. Although skin cancer can occur at even a young age, it is important to exercise particular caution in assessing new moles or skin lesions in patients over 50. If such a patient presents with a mole that clinically may otherwise look benign, but has appeared at this age as a new lesion, do consider malignancy. Single lesions should also make you exercise caution – if you are presented with a single nodule, a single persistent red scaly patch, or a single actinic keratosis, always consider a histological diagnosis.
8 Up to 5% of melanomas are amelanotic
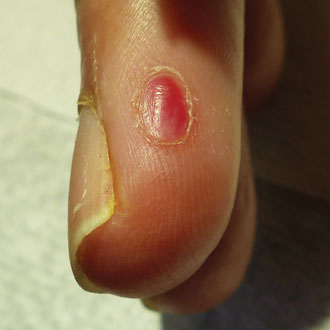
Up to 5% of melanomas are amelanotic (pink melanomas), and can mimic pyogenic granuloma. Suspicious features may include no history of injury, a lesion arising from the distal nail, or one with anything atypical at its base, such as vessels or pigmentation. Any fast-growing pink nodule merits a two-week wait referral; in some parts of the country some dermatology units now advise that best practice is for all pyogenic granulomas to be referred by two-week wait. All such lesions should have at the very least ‘soon’ excision, and any ‘pyogenic granuloma’ that is atypical in any way, or arising in an older person, should be referred urgently to exclude pink melanoma.
9 Facial melanoma can be slow growing, and the nose, ears and lips are high-risk sites for skin cancer
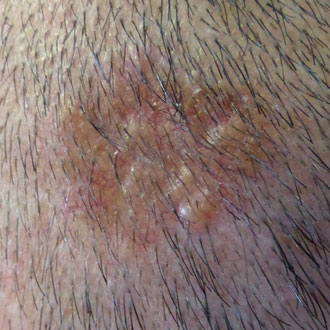
Melanoma on the face can be slower growing than other body sites. Solar lentigos on the face commonly have an irregular outline, but these lesions should be non-palpable and the brown colour should be regular, even and uniform. If a facial solar lentigo has different shades of brown consider urgent referral to exclude lentigo maligna (melanoma in situ).
Also beware any non-healing lesion on a sun-exposed site. Nodular basal cell carcinomas (BCC) typically have a pearly appearance or edge, but other types include superficial BCCs, which may be a flat, solitary, non-healing red patch, or morphoeic BCCs, which may appear as a white, scar-like area without history of injury. If a skin lesion on the head or neck is not responding to anti-infective treatment, consider malignancy. Also remember that in patients who are HIV positive, BCCs can occur at a younger age, and have a higher risk of recurrence.
10 Remember the risk factors for squamous cell carcinoma (SCC)
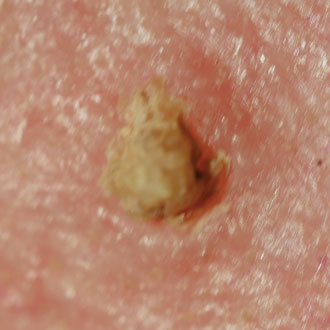
An important risk factor to be aware of is that SCC is more common and more aggressive in the transplant population, or those on immunosuppressant medication. Keratoacanthomas are simply well- differentiated SCCs and all need urgent referral. Around 15% of cutaneous horns have SCC at the base, so if the base is at all thickened these need urgent excision. The lip is a high-risk site for early invasive SCC so if a patient presents with an unexplained white patch of leukoplakia on the lip, consider urgent referral. Chronic lichen sclerosus or lichen planus can give rise to SCC. And remember that any site of previous trauma, not just chronic leg ulcers, can undergo malignant transformation to SCC.
Dr Sara Ritchie is a GPSI in dermatology in Stoke Newington, north London













