How will a booster Covid vaccine programme look for GPs?
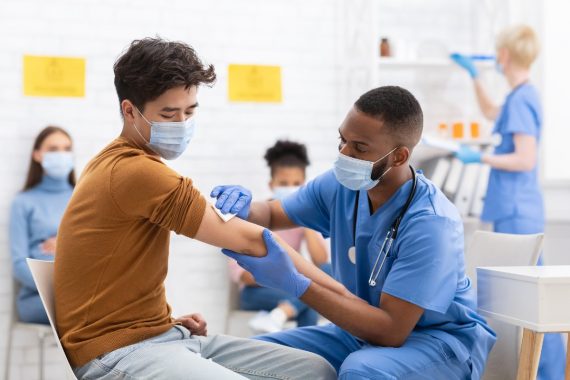
As a programme is lined up for the autumn, it is still unclear who will receive the jab and which vaccines might be used. Nicola Merrifield asks experts about the behind-the-scenes discussions
GPs have ensured the Covid-19 vaccination programme has so far been a triumph – but may have to do so all over again.
Plans for booster jabs, potentially from the autumn, are in the pipeline. It is likely these would need to ‘dovetail’ with the flu vaccination rollout, and trials are ongoing into the effects of giving different brands for first and second Covid doses, as well as into the safety of vaccinating children.
Last month, vaccines minister Nadhim Zahawi confirmed the earliest possible start for a booster campaign: ‘We will be ready from September onwards, both in terms of giving [the chief medical officers] the vaccine options, but also the NHS team is making plans now.’
Speaking to BBC Radio 4, he added: ‘It may be a month later or two months later. Or the beginning of next year, depending on the clinical decision.
‘But we need to give them that capability because it will need to dovetail with the flu vaccination programme.’
We look at what this might mean for GPs and patients.
What vaccines will be given?
The Government has announced it will trial seven different existing vaccines as boosters to deal with Covid variants.
Last week, the Government launched its ‘Cov-Boost’ trial looking at whether a third shot of the same brand or a different existing vaccine brand would increase immunity, and whether any side-effects are produced. Early results will be published by September to inform the decision on whether an autumn booster campaign goes ahead.
Meanwhile, manufacturers Pfizer, Moderna and AstraZeneca are already accelerating the development of tweaked boosters to combat the variants. Moderna says a version of its jab ‘increased neutralising antibody response’ against the Brazilian and South African variants.
But modified versions may not even be required. The existing Pfizer, Moderna and AZ vaccines appear to offer protection against the Kent mutation, and possibly the Brazilian variant, with Pfizer and Moderna also tackling the South African variant.
‘We know B117 [the Kent variant] is effectively controlled by the existing vaccine. The South African strain is probably controlled – maybe not quite as effectively,’ says GP and vaccine expert Dr Peter English.
The early indications look positive around effectiveness against the Indian variant, which the WHO has declared a variant of concern. Health secretary Matt Hancock said on 18 May the variant was ‘not penetrating older, vaccinated groups’. A study by Public Health England, published on 22 May, found both the Pfizer and AZ vaccine offer high levels of protection against symptomatic disease from the Indian variant, following two doses.
If the Government opts to stick with existing vaccines, it must then decide whether to ensure patients stay with their original vaccine brand or can be given an alternative for their third dose.
Dr English suggests there may be more benefit in changing the vaccines. ‘With the long prime boost interval we’ve been using in the UK, we’ve probably got pretty good boosting from the second dose.’
In support of varying brands, he cites ‘particularly strong’ evidence that a DNA vaccine followed up with an antigen vaccine works well for some diseases. No current Covid-19 vaccines are DNA based but these could be developed in future.
The Government-commissioned trial Com-Cov – the precursor to Cov-Boost – launched in February and has looked at interchanging the AZ and Pfizer vaccines. In April, this was extended to include the Moderna and Novavax vaccines.
Early results show mixing Pfizer and AZ vaccines increases the chance of mild/moderate side-effects, such as fatigue or headache, but these reactions have been short lived, with no other safety concerns observed. The study has yet to report on any impact on immune response.
Even if immunity is not improved, the flexibility afforded will be valuable, says Dr Raghib Ali, senior clinical research associate at the University of Cambridge’s MRC epidemiology unit.
‘It’s likely we’ll be able to interchange vaccines… when we get to that stage you’ll be given whichever is available.’
How will it be delivered?
GPs delivering vaccines at their own practices is not widespread, despite NHS England guidance in January permitting this for the AZ vaccine. But many GPs do want to do it as standard.
At last month’s UK LMCs conference, a successful motion from Waltham Forest LMC called on the BMA’s GP Committee to ‘proactively negotiate with NHS/DHSC a direct enhanced service so that if an annual Covid-19 vaccination programme is required it will be contracted with and delivered by individual general practices’.
Meanwhile, Pulse’s latest survey reveals 58% of 260 GPs in England who are not currently vaccinating patients at their own surgeries would like to do so.
Professor Linda Bauld, a public health policy expert and behavioural scientist at the University of Edinburgh, says this benefits patients: ‘It is better for patients to go to a practice they are familiar with, particularly the older and more vulnerable groups.’
During a House of Commons debate in April, health secretary Matt Hancock was asked why this wasn’t possible. Mr Hancock replied: ‘That is the first I have heard of that concern. I will take it away and ensure it is looked at properly.’
The MHRA last week authorised an extension of the storage time for the Pfizer vaccine at fridge temperature, meaning it can now be kept at +2 to -8C for a month – up from five days. NHS England said the ‘additional flexibility’ would make it easier to plan vaccine clinics and pop-up vaccination sites.
Moving Covid-19 vaccination to practice level would also make it easier to deliver flu jabs at the same time – an approach ministers appear keen on.
Of 398 England-based GP partners responding to Pulse’s survey, 80% said they wanted to be able to administer the two jabs together at their own practice.
A Government-funded study looking at the co-administration of flu and Covid vaccines is in its early stages. Experts say it’s not clear if the JCVI will authorise it this year or await more evidence.
Dr David Strain, a consultant in older adults’ medicine and clinical lead for Covid at the Royal Devon and Exeter Hospital, is working with flu vaccine manufacturers on co-administration.
Two companies are currently looking at combining the vaccines in one shot, he says. ‘That would be akin to MMR – one injection, three antigens – you’d produce a response to three different things.’
However, MMR uses the same technologies. None of the current flu vaccines matches up with the way Covid vaccines are built (either using mRNA – as with Pfizer and Moderna – or adenovirus, as with the AZ vaccine).
‘So we are looking at two different technologies. We don’t even know if we’ll be able to use the same adenoviral virus vectors next year as we don’t know if people will become immune to those, which could reduce vaccine effectiveness.’
Theoretically it would be possible to combine different technologies in the same jab, says Dr Strain, as long as they are kept at the correct temperature and don’t interact – which is ‘the biggest risk’.
The other option would be for GPs to give the flu jab in one arm and the Covid jab in the other, which would also help identify which vaccine caused any reactions observed, says Dr English.
But Dr Strain warns it is possible the flu vaccine could cancel out the effects of the Covid vaccine if co-administered.
‘If your immune system suddenly becomes stimulated by the flu and you get the typical fever quickly – would that trigger you to wipe out [AZ’s] chimpanzee adenovirus before it has had a chance to produce the coronavirus protein?’
Who will receive the jabs?
The Covid vaccination programme has so far been limited to adults but children could be included as early as August in the UK, according to some reports.
The UK trial of AZ vaccination in children was paused in April following blood clot scares, but Pfizer’s vaccine was approved earlier this month by the US regulator for use in 12- to 15-year-olds, with trials ongoing for children aged six months to 11 years old. Moderna is also testing its vaccine with children aged six months to 12 years.
If the UK is to achieve herd immunity children will need to be vaccinated, as they ‘are probably more transmitters than adults because they mix with so many more people’, says Dr English.
‘There’s quite good evidence for the adolescents… I’ve no doubt children will follow. [One reason] is some do get long Covid and prolonged illness, although they are far less likely to die.’
Immunosuppressed patients are also being investigated more closely. Dr Strain says: ‘We know in that population that the T-cell responses are not strong so theoretically all we’d need to do is give them a booster of the same jab they’ve already had, remind their T cells there is something coming towards them, so if they get infected the T cells are ready.’
As for the rest of the UK population, England’s chief medical officer Professor Chris Whitty has hinted that a booster campaign from the autumn may be limited to the top priority groups.
However, there is no certainty a booster vaccine will be needed this year. Professor Whitty said in February that two factors would decide whether revaccination was required: vaccine-resistant variants and waning immunity.
Dr English says there is ‘minimal evidence’ that people’s immunity will have decreased by the autumn, even for those who were vaccinated earliest.
Dr Strain adds: ‘If I was a betting man I’d put money on the average population not being likely to need a booster until autumn 2022.’
A booster campaign for the vulnerable this year would be more of a precaution, he adds: ‘For this winter I would realistically expect the vulnerable, the elderly and the immunocompromised will need a booster.
‘That will be more about erring on the safe side – we don’t want to wait until we have entire nursing homes dropping dead before we decide to do something.’
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.














