NICE recommends GPs use FIT test for all suspected colorectal cancer patients
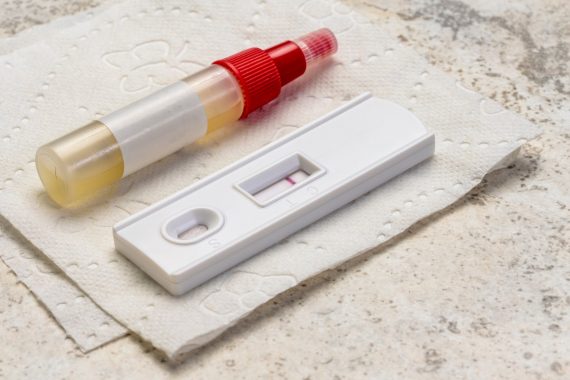
NICE has recommended that GPs use FIT tests to triage all patients with signs or symptoms of colorectal cancer in a bid to reduce colonoscopy waiting times.
In draft guidance that has been released for consultation today, NICE said that people with results of 10 or more micrograms of haemoglobin in their faeces should be referred on for further investigation.
The diagnostic advisory committee has estimated that implementing this guidance could lead to 50% fewer GP referrals for urgent colonoscopies every year.
However, the committee highlighted the importance of continuing to allow GPs to refer people without the required FIT result ‘if they think it is necessary and where symptoms persist’.
The specific quantitative FIT tests recommended for use are the HM-JACKarc or OC-Sensor.
Currently, GPs offer a FIT test to some patients presenting with symptoms indicating potential colorectal cancer, while others are immediately referred on the suspected cancer pathway.
Under this new draft guidance, which will be open to consultation until 19 July, all such patients will receive a FIT test.
FIT tests can correctly identify about 90% of people with colorectal cancer, according to NICE.
NICE’s interim director of medical technology and digital evaluation Mark Chapman said this recommendation ‘could identify people who are most likely to have a condition that would be detected by colonoscopy’.
He said: ‘Introducing FIT to people as an initial test will also mean that those who are unlikely to have colorectal cancer may avoid having a colonoscopy, and those who are more likely to have it can be prioritised.
‘We hope this will reduce waiting times because fewer people will be receiving a colonoscopy they don’t need.
‘These recommendations ensure we are balancing the best care with value for money, while at the same time delivering both for individuals and society as a whole.’
Final recommendations for the NHS in England and Wales will be made after the consultation period has ended and feedback has been reviewed by the committee.
Commenting on the draft guideline, Kevin Barrett, GP partner in Hertfordshire and committee member of the Primary Care Society for Gastroenterology, said: ‘This is welcome news for the healthcare system and the majority of patients who can be strongly reassured by a negative FIT test and saved having an unnecessary colonoscopy, as well as speeding up access to colonoscopy for those patients who are more likely to need one.
‘However, this relies upon patients understanding how to complete the test correctly and doing the test in a timely manner. Maintaining a register of tests given out and results returned is an extra burden on primary care which does not appear to have been taken into account when issuing this guidance. There must be a robust system of safety-netting for patients whose symptoms persist or change after a negative FIT, and also a clear pathway for those who cannot or will not do a FIT test themselves for whatever reason.’
This new recommendation was hinted at in April when Pulse revealed that NICE was expected to update its bowel cancer referral guidelines in the autumn to incorporate triage with FIT testing.
Last year, new guidance from the Association of Coloproctology of Great Britain & Ireland (ACPGBI) and the British Society of Gastroenterology (BSG) advised GPs to downgrade some urgent colorectal cancer referrals based on new FIT thresholds.
The guidance said that patients with a FIT test result below fHb 10μg Hb/g should not be referred via the urgent cancer pathway even if their symptoms fulfil NICE criteria.
Following this, NHS England urged all GPs to implement the guideline’s recommendations in full and said that GPs should manage certain patients with advice and guidance (A&G) from secondary care colleagues.
Pulse July survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.
Related Articles
READERS' COMMENTS [3]
Please note, only GPs are permitted to add comments to articles











There are caveats that need factoring in a) patient test compliance & competence to complete b) patient doing test promptly c) results turnaround time d) Do we mean FIT with bleeding as part of symptomatology or in case of rectal mass when isn’t that helpful/indicated? e) thought QOF was 80% not 100% f) and most importantly is robust management/safety netting/follow up of FIT -ve
FIT tests arent fit for purpose
Cancer Research UK data, shows failure rate 8-18% (depending on where your lab sets its criteria)
I cant see how they refuse to see someone, based on a test with such high error rates!
Any possibility slight clarification Eliza, you are reporting NICE views from their published guidance, but it appears you had the opportunity to directly question Kevin. Both expert views assume the traditional pathway, patient books in to see GP, and then is referred
However this test is widely and cheaply available, indeed one reviewer on Amazon, regards it as so cheap he intends to do one every six months.Wheres the test has a high sensitivity and specificity, certainly relative to FOB, available aisle 3 Tesco ,at that rate I would have thought false positives would become a major issue. The experts do not appear to have addressed this question. What is the NICE guidance with regard to a symptomless positive FIT.