GPs should refer patients who have a suspected allergic reaction to a drug for specialist assessment, according to new draft NICE guidance.
NICE says most patients with drug allergies are not being managed in specialist allergy centres, and their management varies considerably as a result.
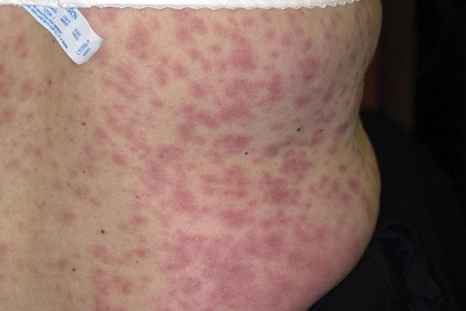
The new guidance – the first of its kind – proposes that GPs should refer anyone who has had a suspected anaphylactic reaction to a drug for specialist assessment, as well as anyone with a severe, non-immediate cutaneous reaction, such as a drug reaction with eosinophilia and systemic symptoms, Stevens-Johnson syndrome, or toxic epidermal necrolysis.
GPs should also refer anyone with suspected allergy to beta-lactam antibiotics who needs treatment that can only be treated by such antibiotics, or who has a high likelihood of needing them frequently in the future, for example as a result of immune deficiency.
And they are urged to ensure that patients are aware of any drugs or drug classes they need to avoid – and that they should check with a pharmacist before taking any over-the-counter drugs.
The guidelines advisors say diagnosing drug allergy is challenging and there is currently wide variation in how it is managed and how easy it is to access specialist services, leading to under diagnosis, misdiagnosis and self diagnosis.
Professor Mark Baker, director of the Centre for Clinical Practice at NICE, said: ‘Hospital admissions for drug allergies are increasing and unfortunately over a fifth of patients with a known allergy will suffer serious harm, or in a small number of cases may even die, because they were given that drug again.
‘This draft guidance urges all healthcare professionals to be alert to the possibility of allergies when administering drugs and provides recommendations on how to properly take heed of them, so that people can be spared from further harm.’