NHS plans set to pour £1.2bn into supporting general practice

Exclusive Blueprints for the future of the NHS are investing more than £1bn into primary care, a Pulse analysis has revealed.
The analysis of the ‘sustainability and transformation plans’ has found that 14 have proposed investment to support the GP Forward View, totalling £394m; extrapolated across the whole of England, this would come to almost £1.2bn.
The Hampshire and the Isle of Wight, and Sussex and East Surrey plans identify the greatest investment in the Forward View, at £71.5m and £51m respectively, with the former specifying delivery of seven-day access, extending the primary care team and offering more specialist care in primary care settings.
Other than this, there is little detail about how the investment will be used. This information is expected to be part of the primary care strategies CCGs had to submit to NHS England by 23 December.
At the same time, the 44 STP ‘footprints’ have to identify £22bn in savings from the health and social care budget between them.
At the start of 2016 NHS England tasked regional teams, CCGs, trusts and councils to produce plans for delivery of the NHS Five Year Forward View, and said they had to make provisions to invest more in primary care.
Two councils in England have rejected their local STP because of its failure to pledge sufficient investment in general practice.
Shropshire Council and Telford and Wrekin Council in the West Midlands said the Shropshire and Telford and Wrekin STP, which predicts a deficit of £131.4m by 2021, should put ‘significantly more resources’ into primary care. Instead, it sets out plans to reconfigure hospital services.
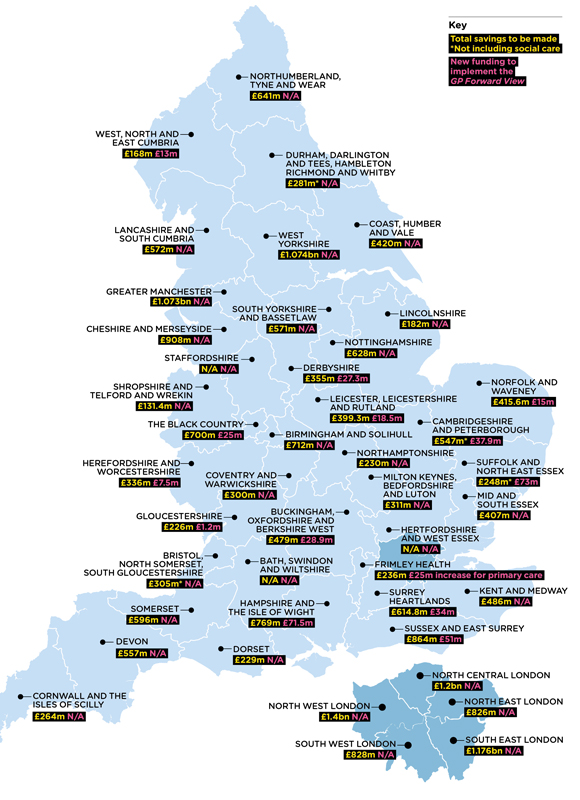
p26 jan 2017 map 580x800px
What are the sustainability and transformation plans proposing?
Pulse’s scrutiny of the 44 STPs have previously revealed how
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens










