Exclusive The Government’s £2.4bn general practice rescue package has failed to relieve GP workload two years on, a Pulse survey has shown.
Asked whether their workload had improved or worsened since the General Practice Forward View was announced in April 2016, eight in 10 GPs (83%) said it had actually worsened.
The survey, which saw responses from 741 GPs, further showed that practice finances had deteriorated for well over half (57%) of respondents, while a similar number (55%) said their staff numbers had decreased.
As a result, nearly three-quarters (71%) of GPs experienced a decline in morale since the GPFV announcement, the poll found.
At the time of the announcement of the GPFV, which contained plans to improve on all of these aspects, NHS England chief executive Simon Stevens promised it would ‘turn general practice around’.
It comes one year after the RCGP – a staunch supporter of the GPFV initiative – ‘red-rated’ several aspects of NHS England’s work to roll out the support.
At the time, RCGP chair Professor Helen Stokes-Lampard expressed ‘frustration’ that GPs were not seeing benefits.
And, commenting on Pulse’s survey results, she said: ‘We’re now almost two years into NHS England’s five-year GP Forward View and, particularly around workforce issues, we’d have expected to be further on in its delivery than we are now’.
‘The College is acutely aware of the resource and workforce pressures facing general practice, and we are committed to holding the Government and NHS England to account to deliver the GP Forward View in full, as a matter of urgency.
‘There is a huge amount of work left to do to deliver the GP Forward View – but the plan remains the best, and indeed the only, chance we have of turning things around for general practice. Only when its pledges are fully delivered will we be able to ensure the high-quality care our patients need, and deserve, both now and in the future.’
The BMA recently warned that ‘very little’ of the funding pledged in the plan had been delivered, with bureaucracy over accessing small pots of funding acting as a hurdle to practices benefitting from the package.
The chair of the BMA’s GP Committee Dr Richard Vautrey told Pulse that the survey findings ‘chime with what our own members tell us about the pressures they are facing on a daily basis’.
According to Dr Vautrey, GPs ‘struggle with rising workloads, staff shortages, dwindling budgets and low morale while trying to meet the health needs of a growing population’.
‘It’s a sign of the scale of the problem that the commitments made in the GPFV are yet to make tangible improvements to the day-to-day experience of GPs and practices,’ he said.
Dr Vautrey said the BMA is now calling on NHS England to ‘go beyond the commitments in the GPFV’ and deliver ‘proper recurrent investment and an expansion of the workforce in and around practices that will be able to address the pressures in general practice’.
The calls come as the BMA recently published an updated version of its demands to NHS England, titled Saving General Practice, following the failure of the Government to deliver on the demands of the BMA’s Urgent Prescription for General Practice in 2016.
On workload, the document demands that practices are enabled to manage their workloads to protect patient safety. It further calls on the Government to retain the core GP contract, expand the workforce, provide a fully funded indemnity package and provide recurrent, sustainable funding for practices.
NHS England said that there are more than 2,300 more practice staff providing direct care, while 2,100 practices have been directly supported via the GP practice resilience fund.
A spokesperson said: ‘This is a tiny and self-selecting survey which lacks statistical credibility.’
The GPFV promised to deliver an additional investment of £2.4bn a year by 2020/21 into general practice services, bringing it to a total of £12bn.
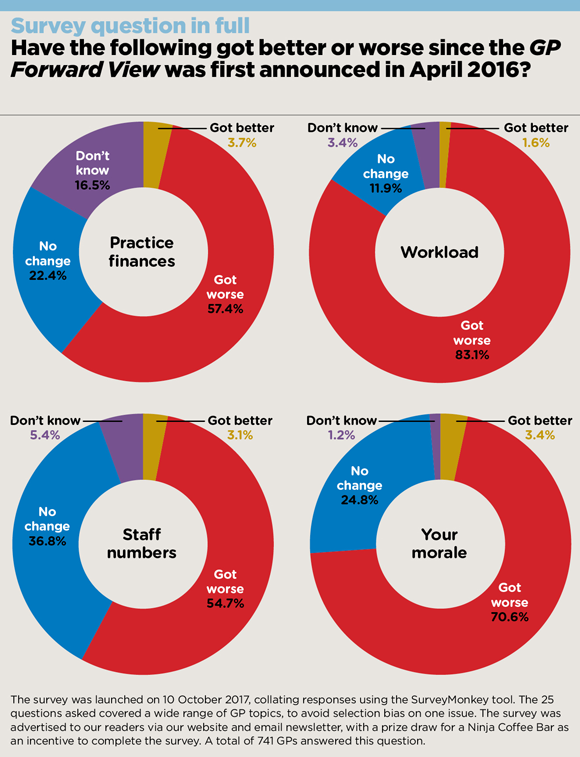
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens












