Revealed: GP vacancy rates rocket with one in six roles unfilled

Exclusive GP vacancy rates are at the highest level ever recorded, with one in six positions currently unfilled, a major Pulse survey has revealed.
Pulse’s annual vacancy survey of 658 GPs found that 15.3% of GP positions are currently empty, up from 12.2% last year, and 11.7% in 2016.
It also showed that the recruitments issues were concentrated on certain practices, with two-thirds of the vacancies reported at practices where there were more than one position unfilled.
GP leaders said that these workforce shortages are ‘placing an intolerable pressure’ on GPs.
The last official figures were published in 2011 and showed a 2.1% vacancy rate. Pulse has run its vacancy survey since 2012, when the level of positions vacant was 4.2%, and it offers the only longitudinal data on the subject.
GPs reported that inability to recruit and funding shortages have also forced many practices to cut GP positions, relying on non-GP staff and forcing practices to close patient lists.
Recent official figures showed that 1,000 GPs have left the workforce since 2015, setting the Government well behind its target to recruit 5,000 GPs by 2020.This caused health secretary Jeremy Hunt to admit that fulfilling the target would be a ‘struggle’.
In January, the BMA revealed that almost half of GPs had vacancies in their practices. This comes after a third of GP practices told the BMA they had vacancies unfilled for 12 months, and nine out of ten said their workload was often unmanageable.
Dr Janine O’Kane, a GP partner in Belfast, said her practice can no longer afford more doctors and also relies on her nurse practitioner. Dr O’Kane said: ‘They are starving the best and most cost effective primary health care system in the world of funds.’
Another GP, who did not want to be named, said failure to recruit GPs has forced them to rely on nurse practitioners, pharmacists and paramedics.
He said: ‘This provides appointments but means that individual GP list sizes have risen substantially. Results, letters, paperwork, prescribing requests and admin workload all go to the named GP, so high list sizes bring high workload and responsibility.’
The shift from partners and salaried GPs to a multi-disciplinary team and locums was noted by many respondents. GPs said that advertising for roles resulted in no applicants and one person noted it had taken 18 months to recruit a partner.
BMA GPC chair Dr Richard Vautrey said: ‘The fact that so many surgeries are unable to recruit GPs provides yet more evidence of the scale of the crisis impacting general practice.
‘The Government must prioritise general practice and urgently invest in it to address this growing crisis which is threatening to undermine the foundation on which the wider NHS is built. We cannot allow a situation where patient safety is being compromised by a lack of political action.’
Dr Vautrey said unfilled vacancies have created ‘unmanageable’ workloads.
He added: ‘This is placing an intolerable pressure on local GP services, especially as they increasingly need to deliver intensive, specialist care in the community to the growing number of older patients with complex health conditions.’
RCGP chair Professor Helen Stokes-Lampard said:‘We are acutely aware that GPs and their teams are struggling to recruit across the UK, and the problem is still getting worse. When a practice can’t recruit, they often have no choice but to rely on locum staff, at a greater cost.
‘We know that in some areas recruiting locums is becoming difficult, and we are short of other allied healthcare professionals in the community too – especially experienced practice nursing staff. The problem is that in many areas the GPs simply aren’t there to employ.’
A Department of Health and Social Care spokesperson said: ‘GPs are a crucial part of the NHS – that’s why we are increasing investment by £2.4bn a year by 2020 and more than 3,000 GPs are expected to be recruited into training this year.
‘The Prime Minister recently announced increased funding for the NHS by £20.5bn over the next five years – to secure the future of the health service as it celebrates its 70th birthday and ensure we can deal with the pressures of a growing ageing population.’
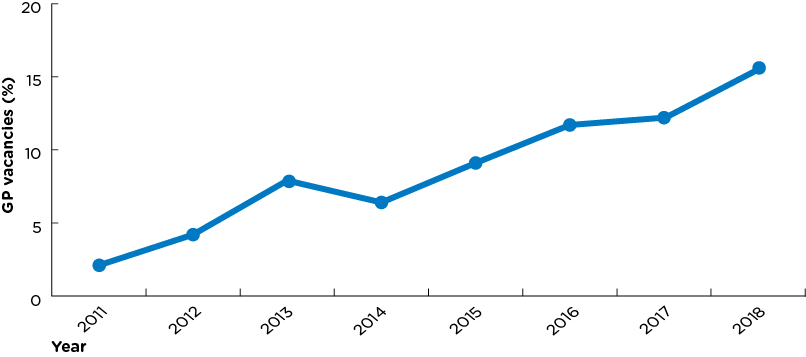
vacancy rates graph









