Small GP practices least likely to receive NHS England resilience funding

Exclusive Small GP practices are least likely to receive NHS England resilience funding, despite accounting for the majority of closures over recent years, Pulse can reveal.
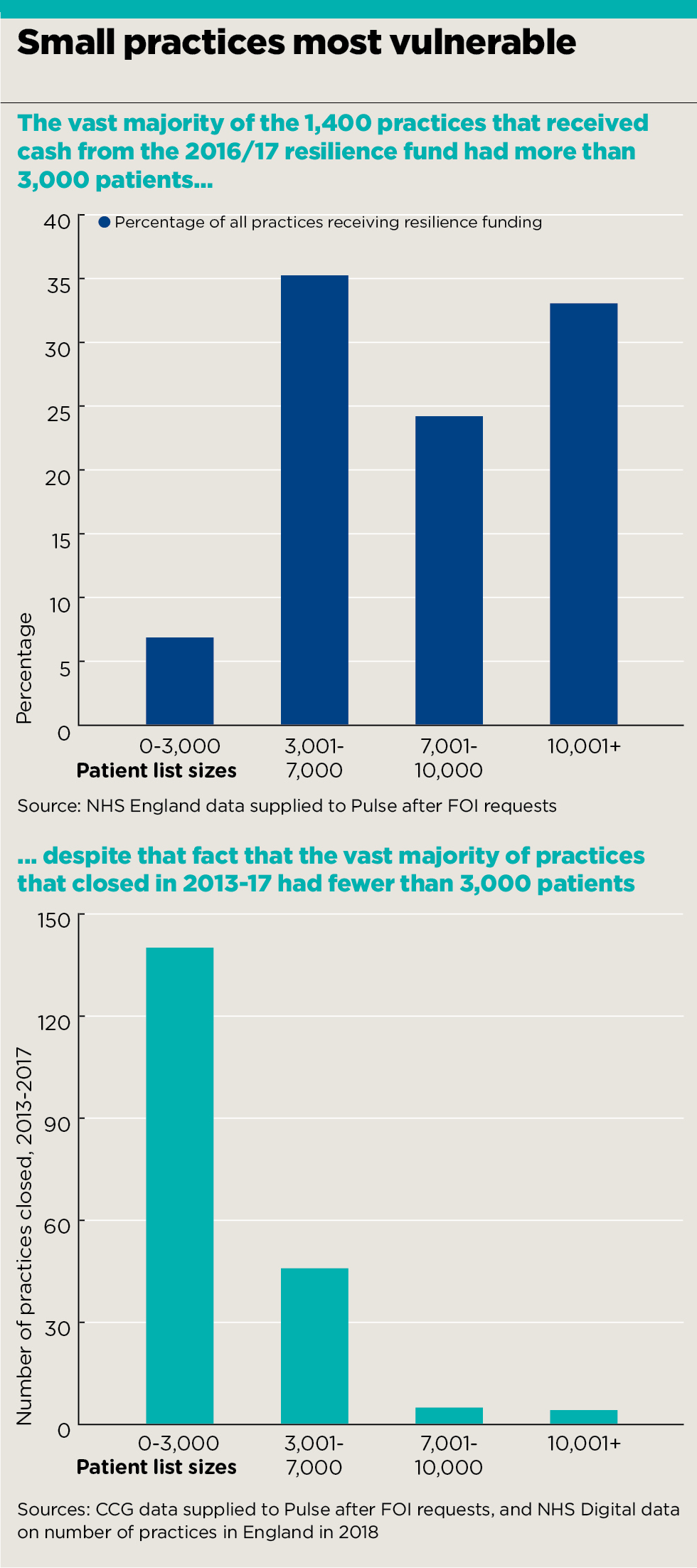
Only 7% of all practices that received cash from the £16m of the General Practice Resilience Programme allocated in 2016/17 served populations of fewer than 3,000 patients, according to NHS England data supplied to Pulse following a freedom of information request.
Overall, such practices make up around 10% of all practices in England. But a separate FOI to CCGs showed the vast majority of practices that closed in 2016 and 2017 – 76% – were small, with a similar trend between 2013 and 2015.
NHS England has claimed it has since increased funding for smaller practices.
This comes after Pulse ran comments by NHS England’s top GP, Dr Arvind Madan, suggesting GPs should be ‘pleased’ when small practices close, as there are ‘too many’ of them struggling to meet patient demand. Dr Madan resigned shortly after publication of the interview.
GP leaders said the point of the resilience fund is to help prevent practice closures, meaning a higher percentage of small practices should be benefiting. The latest figures suggest NHS England is supporting larger vulnerable practices ahead of smaller ones, they added.
Data from CCGs show that in 2016 and 2017 a total of 81 small practices had to shut their doors. Over the same period, just 22 medium-sized practices (3,001 – 7,000 patients), and three large practices (7,001 or more patients) closed.
Despite this, a far higher number of larger practices were allocated resilience funding than smaller ones.
resilience funding data
NHS England guidance says the funding pot totalling £40m to be distributed over four years is aimed at supporting practices ‘to become more sustainable and resilient, better placed to tackle the challenges they face now and into the future’.
Although the figures were provided by NHS England, after Pulse’s FOI request, a spokesperson said: ‘This cherry-picked data does not reflect a true picture of resilience funding provided to small GP practices. We are continuing to help practices that need it most, with more than 3,000 packages of support provided to GPs with list sizes of up to 7,000 in 2017/18, up from nearly 600 in 2016/17.’
But GP leaders have expressed concern at how resilience funding is allocated.
Dr Matt Mayer, the BMA’s GP Committee regional representative, and CEO elect of Berkshire, Buckinghamshire and Oxfordshire LMC, said: ‘These statistics are deeply concerning. The fact that much-needed resilience funding is least likely to get to those practices that need it most illustrates that the GP Forward View is not fit for purpose, and is simply window dressing.’
He said this reinforced concerns voiced by grassroots GPs – following Dr Madan’s comments – that NHS England is ‘not serious about supporting local, small-scale, traditional general practice’ and prioritises larger practices instead.
Dr Mayer called for an end to the ‘Kafkaesque process’ of GPs having to bid for various pots of money to sustain basic services. He said core GP funding needed ‘urgent’ uplifting, adding: ‘Small practices need real financial support which is not contingent on the ever-increasing push to work at scale.’
GP Survival chair Dr Alan Woodall, a GP in Powys, said: ‘NHS England must answer how it is that the most vulnerable practices, requiring the most help to stay viable, have received the least funding.
‘Is it because they haven’t applied because they weren’t aware, or that they have and the system has discriminated against them? Or is the system so full of red tape they lack the capacity to do it?
‘If more smaller practices received this money, the chances of them being able to recruit, and look attractive to partners or salaried GPs, would rise – and it would make them more stable,’ he said.
In Pulse’s interview last month, Dr Madan stood by comments he had made stating ‘most businesses are pleased to see rationalisation of providers’, which he linked to small practices closing.
He has since resigned, after admitting he had been posting provocative comments under the pseudonym ‘Devil’s Advocate’ on the Pulse Today website.
The Arvind Madan small practices scandal
The comment at the heart of the scandal that saw NHS England primary care director Dr Arvind Madan resign his post came in response to a Pulse investigation which revealed that 450 GP surgeries had closed between 2013 and 2017.
Posting under the pseudonym Devil’s Advocate, Dr Madan said: ‘Most businesses would be pleased to see a rationalisation of their markets, as it makes the remainder more viable. This happens in all markets.
‘Lets face it, there are probably too many small practices out there struggling to do everything you would want for your family in an era of modern general practice.’
Although Dr Madan’s resignation statement said he wanted to ‘make it categorically clear that these comments are not a reflection of NHS England policy’, the latest data uncovered by Pulse shows that smaller practices are not getting the same funding as large ones.
Following the resignation of Dr Madan, NHS England has yet to prove that it is supportive of small GP practices which, through circumstances often beyond their control, struggle to fit into NHS England boss Simon Stevens’ Forward View agenda.














