A 39-year-old man presents to his GP with sudden onset severe pain in the left shoulder and arm, following a recent episode of influenza. The gentleman gives no history of trauma and has not had any previous surgery to the shoulder, neck, axilla or thoracic region. He is otherwise fit and well.
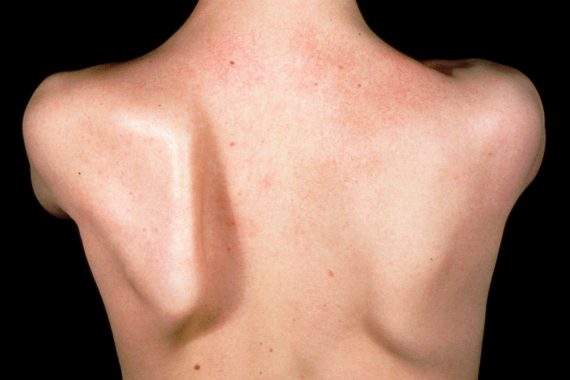
Clinical examination reveals a normal cervical spine, with a good range of motion. On closer examination of the left shoulder, any movement is painful. A winging of the left scapula is also noted. Examination of the left elbow, wrist and hand is normal.
The GP organises an initial investigation of simple blood tests, which reveals a normal FBC and inflammatory markers, while shoulder and scapular radiographs do not reveal any bone injury.
The patient is then referred to an orthopaedic surgeon for a second opinion, and further investigations are made on a routine basis. Further complex investigations include MRIs of the left shoulder, cervical spine and brachial plexus to rule out other sinister pathology are performed. Characteristic MRI findings show denervation changes in the patient’s muscles, and an electromyogram and nerve conduction studies confirm brachial neuritis.
The patient is started on a course of corticosteroids, opiate analgesics, as well as intensive physiotherapy.
The problem
The shoulder girdle is comprised of the clavicle and scapula, which allows articulation of the humerus at the glenohumeral (GH) joint. The scapula maintains dynamic stability of the GH joint, in addition to providing a stable base for muscular attachments.
Winging of the scapula manifests when there is pathology affecting the muscles of the shoulder girdle or the nerves supplying it. It causes significant functional problems such as weakness, decreased elevation of the affected arm and pain, or to a lesser degree, a cosmetic deformity.
Causes:
Iatrogenic
This can be through injury to the long thoracic nerve supplying the serratus anterior during axillary clearance in breast surgery, causing medial winging of the scapula.
Alternatively, this may be through damage to the spinal accessory nerve supplying the trapezius, acquired during surgery or from radiation to the posterior triangle of the neck, causing lateral winging of the scapula.
Trauma
This is a result of scapula or clavicle fractures, or acromioclavicular joint disruptions. This can be secondary to pain, causing abnormal shoulder movements, or direct trauma to the muscles or nerves supplying the scapular-stabilising muscles.
Inflammatory
There are post-viral causes associated with brachial neuritis.
Muscle pattern shoulder instability
This is a common cause, leading to scapular dysrhythmia and subsequent winging.
Parsonage-Turner syndrome
Also known as brachial neuritis, this can lead to weakness of the scapula muscles. The syndrome is idiopathic in the majority of cases, however, many specific risk factors have been identified, such as post-operative, post-infection, post-traumatic or post-vaccination.
Primary muscular dystrophies
Primary muscular dystrophies can be a rare cause, seen in facioscapulohumeral dystrophy (FSHD), which affects the scapular stabilising muscles. FSHD is an autosomal dominant disorder in as many as 90% of affected patients. Shoulder weakness is the presenting symptom in more than 82% of patients with symptoms.
Features of condition
Patients present with impaired function in the form of reduced elevation of the affected arm, sometimes accompanied by pain. There is also a cosmetic defect which can sometimes be quite prominent.
Examination
- Initial inspection may reveal previous surgical scars from axillary clearance in breast surgery or previous neck or thoracic surgery.
- There will be an asymmetrical posture of the shoulders.
- Posteriorly, a winged scapula protrudes further out compared to the normal side. The ‘wall push’ test, where the patient pushes with the arm outstretched against a wall, can make the winged scapula more prominent
Treatment
The management of a winged scapula is dependent on the cause, and can be divided into two treatment categories: operative and non-operative.
Most patients require non-operative supportive treatment like analgesia and physiotherapy, although recovery can take up to two years in some cases.
Rarely, patients require operative treatments when non-operative measures have not succeeded, such as:
- Neurolysis for pain control
- Nerve repair
- Nerve transfers – for example, to the serratus anterior muscle
- Dynamic muscle transfers, such as a pectoralis major transfer
- Surgical stabilisation of the scapula – for example, scapulopexy (fixation to the chest wall or spinous process of the vertebrae) or scapulothoracic arthrodesis to help with pain.
Mr Ali Noorani is a consultant orthopaedic and trauma surgeon at St Bartholomew’s and Royal London Hospital.
Miss Suan Khoor is an orthopaedic registrar at the Royal London Hospital
Mr Sirat Khan is an orthopaedic registrar at the Royal London Hospital
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens