A day lasering away tattoos
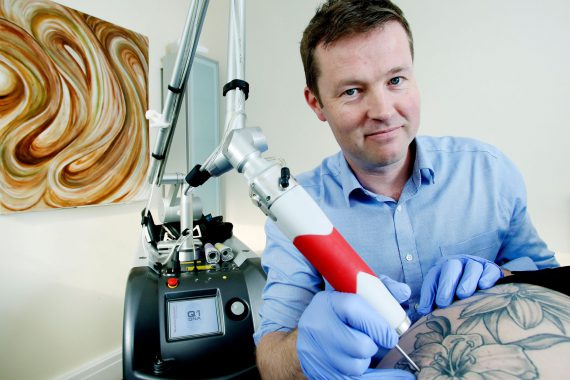
Profile: Dr Ben Mills

Age 44
Role GP partner and director of a laser tattoo removal company
Tattoo removal training Manchester University spin-off company
Location Derby
Hours worked per week Three days a week as a GP partner, two days a week doing laser tattoo removal
09.30
I arrive at the clinic after the school run. It is a room in a hairdresser and beauty salon, with laser warning signs and a lockable door. I prepare the surfaces, draw up syringes of local anaesthetic and dig out that day’s patient treatment cards.
I started four years ago after patients asked for advice about safe tattoo removal. This led me to the deregulated world of laser treatment. There is no standardisation of equipment or training, meaning it’s a lottery for those trying to remove their unloved ink. As with tattooing itself, cheap equipment from overseas is available so that anyone and everyone can ‘have a go’. But a common mistake made by DIYers is overtreating so that the skin cooks and scars.
10.00
My first patient comes in. She has three tattoos – on her ankle, abdomen and shoulder. Only a handful of patients have just the one tattoo.
I check on any problems with the previous treatment and ask about any health changes. We might compare the treatment area with the pretreatment photo. Progress is never as fast as they hope but I’m very clear at the outset that it’s likely to take a couple of years.
I follow my usual steps. I anaesthetise the area, then laser it and apply an ice pack. The anaesthetic and post-treatment swelling limit how big an area we can treat in a session. As a GP I can offer local anaesthetic, which makes a massive difference – I speak from experience as I had a tattoo put on my leg so I could ‘practise’ removing it. It wasn’t until then that I realised how painful the process is.
10.30
One of my regulars comes in. I’m slowly lightening the colourful half-sleeve done by her amateur tattooist ex. She tells me that with a bit of fake tan, you can hardly see it. However, this has taken two years.
11.00
I have a new patient. Based on my GP knowledge I can offer a detailed initial consultation to get informed consent – way beyond the photocopied ‘consent forms’ I’ve seen from other providers. My initial consultation and patch test takes an hour – we talk about what a tattoo is, how the laser works, side-effects and potential problems. I check their health and medication history and anything that might make the skin slow to heal or light sensitive. We discuss how the tattoo needs repeated treatments and despite their enthusiasm, not too often. Appointments are typically spaced six weeks apart, although a longer wait is better for the patient.
Most patients expect it’s going to take time, but some want it gone ASAP so they can get a job that requires ‘no visible tattoos’ or before they get married. I have to let them down gently. With today’s patient we select a patch of tattoo, numb it, laser it and ice it. I send them away to let the patch settle and to let them decide if they want to commit to the time, discomfort and expense.
12.00
I answer a couple of email requests for quotes – from homemade tattoos done 30 years ago to a tattoo regretted after just one day. The cost of treatment varies – ranging from hundreds to a few thousand pounds, over a few years.
12.30
I treat my oldest patient, a 73-year-old man who had an embarrassing tattoo put on his chest 50 years ago in a refugee camp. He hasn’t taken his shirt off in public since, but he wants to return to his native hot pools to ease his rheumatism and would like ‘the lady’ gone.
13.00
I have two more patients, both middle-aged men with forearm tattoos. They feel they can’t roll up their sleeves now they are in the boardroom. Both tell me how they are resigned to the fact their kids will get tattoos because of fashion and ease of access. There are at least 10 tattoo parlours within a mile of my clinic.
14.30
I clean up and it’s time to do the school run. Some people love their tattoos and some tattoos are truly works of art. However, the majority don’t and aren’t. Just like my GP job, there’s lots of work.









