The private health checks driving unofficial screening
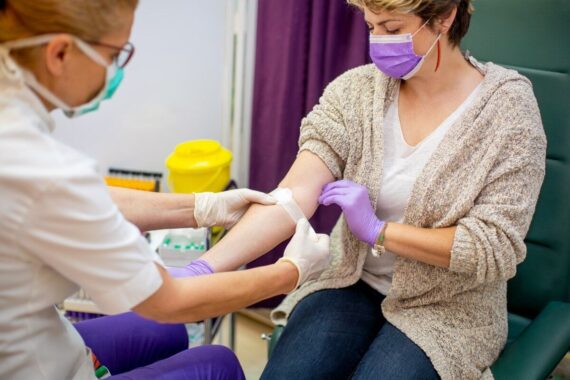
As part of Pulse’s latest series on screening, Emma Wilkinson looks at the take-up of private health checks and how this is affecting GPs
There are numerous companies offering private health screening. These preventive checks can often be done online in the comfort of your home or by attending a clinic. Depending on the package, it could include things like heart rhythm screening, spirometry, a battery of blood tests and urinalysis.
You do not have to have health insurance or a corporate package to access these – although there are big money-off deals. For example health insurance provider Vitality offers members 81% off a Bluecrest Health screen. But customers can also simply purchase a ‘pay as you go’ option, from around £200 for the most basic package, to £900 for the top package.
At Bluecrest Health, people over 40 years can have a cancer risk screening check with HPV tests (for women) and PSA (for men) as well as H. Pylori and FIT testing. Others, including Bupa, restrict PSA to the over 50s but offer a mammogram from 40 years.
Some companies will also do genetic screening for high-risk genes. A GP who wished to remain anonymous told Pulse she had reluctantly received a genetic screen as part of a two-for-one offer taken up by a family member, which unexpectedly identified her as a BRCA2 carrier.
This has led to difficult decisions, ongoing testing and pressure for surgery. ‘It has caused a burden on the family that I’m not sure is worth the knowledge,’ she says.
The take up of private health screening continues to increase. An RCGP survey in 2018 found nine in 10 GPs in the past year had seen a patient to discuss the results of a private health screening. Last year, a Pulse investigation found GPs reporting an increase in patients opting to go private for healthcare during the pandemic. And a 2021 report by health data firm LaingBuisson found NHS waiting times were having a direct impact on the demand for self-pay in a way that ‘hasn’t been seen in recent years’.
Professor Carolyn Chew-Graham, professor of primary care research at Keele University says: ‘Patients come in and say I’ve had my private health check, these are the results can you go through them. I explain that’s the responsibility of the person who organised the tests and they say well I don’t have a follow up. I try and be firm but it is difficult when there are abnormalities.’
She adds: ‘It’s extra work that there’s not very much evidence for. If its blood pressure we can say its fine or it isn’t, but things like vitamin D there’s no evidence for doing it, nor is doing routine thyroid function tests in well young people.”
Professor Chew-Graham also raises questions about whether patients know exactly what they are consenting to when they’re having a battery of tests as part of a private health screen: ‘It does make for really difficult consultations.’
Sheffield GP Dr Tom Holdsworth recalls the case of one young patient who came to see him because of microscopic haematuria picked up at a private annual health check. The patient ended up having a host of extra tests with different specialists [on the NHS], which did not find anything and was eventually referred back to the GP where he was left to reassure her all was fine.
‘She was unlikely to have a serious condition, but once it’s been passed to you by the provider on the health check form, it’s really difficult not to follow this up.’
He adds that following all the investigations, the patient concluded that she might not have her health screening next time: ‘I’d had that in the back of my mind the whole way through the process. There is harm here in the procedures she has been through and the use of resources. It’s privatised profit but socialised risk because as soon as they find anything it’s the NHS picking up the pieces.’
Dr Holdsworth also has concerns about spirometry being used as a screening tool: ‘Quite a lot of the health checks do spirometry and again it will just be passed over to the GP.’
He explains that taking a history and asking about risk factors is a whole consultation, and then you will probably feel obliged to do some other tests, perhaps X-ray and another set of spirometry. But inhis experience people being screened do not have an occupational risk but are office workers with no lung problems.
‘You will potentially get to the stage where you say your spirometry was slightly out but everything else seems normal, don’t worry about it. There is no evidence, as far as I’m aware, for doing lung function testing on people without symptoms and without good reason to feel they might have a problem like COPD.’
Bluecrest and Bupa were approached for comment.
Related Articles
READERS' COMMENTS [4]
Please note, only GPs are permitted to add comments to articles














They seem the testing kit but the last line of the instructions is inevitably ‘follow up with gp’.
Or the catch-all, get out of jail free card, used by endless companies… If anything has or hasn’t happened within 1 Pico second of taking the test, see your doctor!
locally we had a lot of hassle from a company offering to check moles in the street. we were then sent patients with ? MM that had to be referred. It is a brave GP who says it is definitely not MM and our local derm consultants were pulling their hair out with the extra workload.
patients buying kits ‘privately’ as entering that route
so they should clearly be told that any follow-up needed is ‘private’ too
@Rogue 1 – somewhat annoyingly that is not what the NHS approach is. My understanding is if a patient is following a private pathway and then decides they want to switch to NHS care they should be taken over by the NHS and they should continue their pathway from the point they were in their private care.
So someone chooses to have a colonoscopy privately, shows a cancer, they could choose to have the rest of their care on the NHS.
Or they choose to have the operation privately, but then after the operation choose to have the rest of the treatment (chemotherapy or radiotherapy etc) on the NHS.
What they are not allowed to do – is continue splitting their care – so have NHS radiotherapy, but go private for the chemotherapy because they have fancier chairs. But they are certainly allowed to switch completely to NHS care.
The clear difficulty nobody has defined is what happens when they want to switch back to NHS care for an incident which would not have happened on the NHS. So they have had bariatric surgery at the age of 16, with a BMI of 31 and no comorbidities – can they switch back to NHS care for follow up? [For clarity I don’t know any surgeon who would do that!]
Or they have screening private that they would not have been offered on the NHS.
or they have a cosmetic procedure, but it has complications and leaves them with a non-cosmetic problem (like an infection after breast augmentation).