GP Covid jabs better value for money than mass vaccination centres, finds NAO
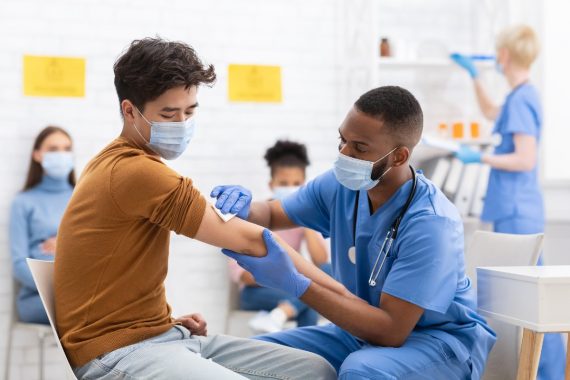
The Covid vaccination programme was an effective use of public money, with GP-administered jabs costing £10 less per item than those given in mass vaccination centres.
Overall, the Covid vaccination programme has vaccinated more people, had less wastage and made greater use of GPs than had been expected when first put in place, the National Audit Office found in an analysis.
The report, which did not include the recent booster programme, found:
- Between the start of the Covid-19 vaccination campaign and the end of October 2021, 87 million doses had been given with 85% of adults having received two doses, far higher than the 75% that had been planned for.
- The number of doses delivered was more than six times that administered in the previous annual flu vaccine and 71% of doses were given by GPs and pharmacists – far above the 56% that had been expected.
- Dedicated vaccination centres have been the most expensive part of the programme at £34 per dose compared with £24 for GPs and community pharmacies.
GPs and community pharmacies were the also the most popular delivery model for all priority groups although people aged under 65 were more likely than others to use dedicated vaccination centres.
And while the programme had planned for 15-20% wastage, only 4% of vaccines had had to be thrown away, which included 1.9 million expiring AstraZeneca doses after changes to clinical advice around their use in the under 40s.
Covid vaccination programme cost £5.6bn by October
The Covid vaccination programme in England has successfully met ‘stretching and unprecedented’ targets and was value for money for taxpayers, the report from the National Audit Office found.
By the end of October 2021, the Covid-19 vaccination programme in England had spent £5.6bn out of total available funding of £8.3 billion for the two years to the end of March 2022, including £2.9bn to purchase vaccines and £2.2bn on deployment.
Contracts or agreements are in place with six suppliers for over 340 million doses of vaccines to be delivered to the UK by the end of 2022, the NAO said.
But the NAO noted that the programme had not met some later objectives including targets to vaccinate most 12-to-15 year olds by late October 2021.
Although there were efforts to address inequalities, the uptake of Covid-19 vaccines in some ethnic minority groups remained substantially below the national average as did uptake in younger age groups and pregnant women.
Yet despite the overall success, there are now substantial risks that must be managed, the NAO concluded, including staffing issues, burnout, and a lack of surplus capacity in the healthcare system.
Gareth Davies, the head of the NAO, said: ‘The vaccine programme has been successful in getting early access to what were brand new Covid-19 vaccines, securing supply of them, and administering them to a large proportion of the population at unprecedented speed.
‘The programme must now redouble its efforts to reach those who are not yet vaccinated while also considering what a more sustainable model will involve as it moves out of its emergency phase.’
Meg Hillier, MP, chair of the committee of public accounts said great credit was due to all those involved from the scientists creating the vaccines to those procuring doses and administering the jabs.
‘However, the success of the roll-out didn’t extend to all parts of society. Government needs to do more to understand how it can better reach those groups and communities where uptake was low.
‘Now the worst of the pandemic has hopefully passed, the government can’t afford to put its feet up. It must learn lessons from its response to Covid to ensure the country is better prepared for future emergencies.’
RCGP vice chair Dr Gary Howsam said GPs and their teams, working with colleagues across the health service, had ‘pulled out all the stops to ensure as many people as possible are protected from Covid-19’.
‘The vaccine rollout was the biggest and most complex vaccination programme in UK history. It also ran alongside two expanded flu vaccination programmes. Its success has in a large part been down to the experience, hard work and dedication of GP teams, delivering vaccinations at a local level, with the majority of vaccinations delivered in primary care.’
He pointed out that the report did not take into account the booster programme, which has now seen more than 38 million patients fully protected.
‘It remains crucial that patients continue to get as much protection as possible so that we can move from a pandemic to an endemic Covid situation and GP teams will remain key to this effort.’
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.
Related Articles
READERS' COMMENTS [10]
Please note, only GPs are permitted to add comments to articles











Ursine faecal matter found in Vatican arboretum by pontiff who remains catholic.
Completely unsurprising.
Alas, NHSE management is ideologically driven.
That ideology believes ‘Hospitals are good. GPs are bad. Management Consultants are good. Central control is good. Autonomy is bad. Power is good. Oversight and accountability are bad.’
No amount of evidence will change their view – it is too entrenched and comfortable for them.
Management culture in the NHS is the problem, not the solution.
Complete reform of management culture and ideology is required – but managers cannot be expected or trusted to recognise this and reform themselves.
Our politicians only listen to the managers, and are not capable of identifying and remedying the problem, alas.
Of course after this is published the NHS has decided that the most cost effective part of the delivery of vaccinations should not be used next time round.
Let’s congratulate NHS primary care teams (general practices and pharmacies) who delivered 71% of the total vaccinations given – much higher than was originally expected. As well as delivering more doses than other NHS sites, primary care teams also dealt with the more complex patients – such as the housebound, people living in care homes, the vaccine hesitant and elderly patients who found it difficult to attend a distant vaccination site.
I just did a cardiology webinar. The ECG showed barn door ST elevation.
8% of GPs said it was normal
20% said it was ST depression.
Some of you might want to get off vaccines and wake up and smell the roses. Get out of your PCN too if you can’t handle whats coming for you.
The most cost effective part of the entire NHS for everything is General Practice because we are underfunded.
But Dr Duffy, ECGs are not core work and not commissioned under GMS.
If a practice chooses to deliver ECGs as a service, usually commissioned as a LCS, then obviously the GP(s) responsible for the service should be able to interpret them.
But perhaps the GPs on the call were not all commissioned to deliver ECGs and therefore were not recently practised at ECG interpretation, having not had to interpret one since their house officer years? They might have been there to learn.
I wonder, would our surgical or dermatology or MH colleagues have fared any better?
Brilliant.
Dr Thymes. With all due respect. If you cannot spot an ST elevation, or complete heart block or asystole or VF (and you’re doing enhanced services or not; that is completely irrelevant), but can give 421 covid vaccines, hug panic attacks and sympathise with IBS, then really, you might as well give up. Because the person will be dead. And your naproxen won’t help. And the court room will be a lonely place, alone. The dermatologist or MH nurse wouldn’t be ordering one under daylight anyway.
Thank you for the respectful reply, Dr Duffy, and for the imaginative re-interpretation of the spelling of my surname. Actually I would hope that I can spot ST elevation as I do still interpret ECGs (though generally not in an acute setting as we are not an emergency service).
Perhaps the best comparison is chest x-rays – I suspect most of us could still make a decent fist of interpreting them despite not having seen one (unreported) in many years, but not all of us because they are an investigation almost exclusively taking place in secondary care.
I believe official NICE-approved advice on managing chest pain is not to delay referral by organising or performing tests in general practice, but to refer in as an emergency. In most cases of ST elevation (or PE or palpitations) a good history and examination is all that is required to make that decision.
Interestingly, ST elevation in an asymptomatic patient carries a high false-positive rate: https://www.dicardiology.com/article/technical-factors-involved-false-positive-ecg-stemi-diagnoses
I still think an Old Skool approach is hard to beat, and there is still room for (properly funded and resourced) vaccines, empathy, and a very occasional (consensual, appropriate, GMC-sanctioned) hug.
Dear Dr Duffy,
in GP land you do not rely on ECGs, or troponin levels, or angiograms, to make the diagnosis of an MI. You go by ‘probable’ symptoms. If they seem indicative of an MI we get out of the way, and call the ambulance.
We do not do ECGs, nor do we interpret them. (Some do, but most don’t). It is a skill that we do not require to do our job. n fact, trying to do something you are not good at, and do not do regularly, would be frowned upon by the GMC. Especially if all it did was delay urgent treatment for a patient.
We do not know how to anaesthetise people, nor do a craniectomy either The list of skills that are not required to function as a GP is long.
Vaccinating the public is a an organisation skill that we need, and it seems that we are very good at it. Cheaper and more efficient.
So, instead of berating (some) GPs for not having a skill that is not required to do our job, you should congratulate your fellow professionals for demonstrating, very clearly, that they are very good at what (they need) to do. But I suspect you won’t.