Revealed: one in seven GPs turns to alcohol and drugs to cope

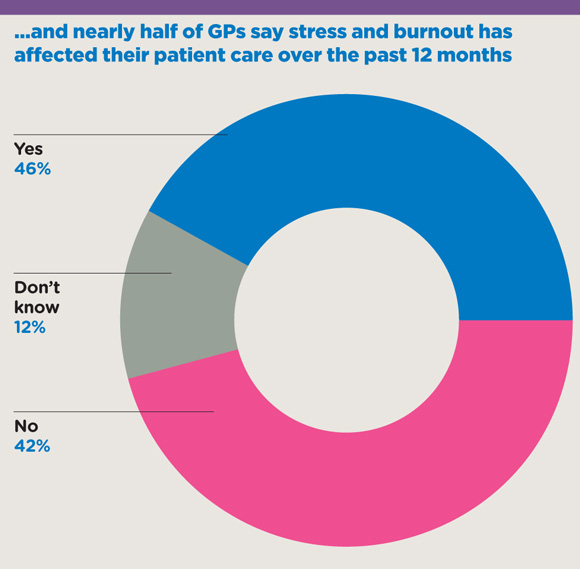
Exclusive Almost half of GPs say their ability to care for patients has been affected by the stress of general practice, a Pulse survey of more than 800 GPs has revealed.
Around one in nine GPs has turned to alcohol because of work pressures, with 6% turning to prescription drugs.
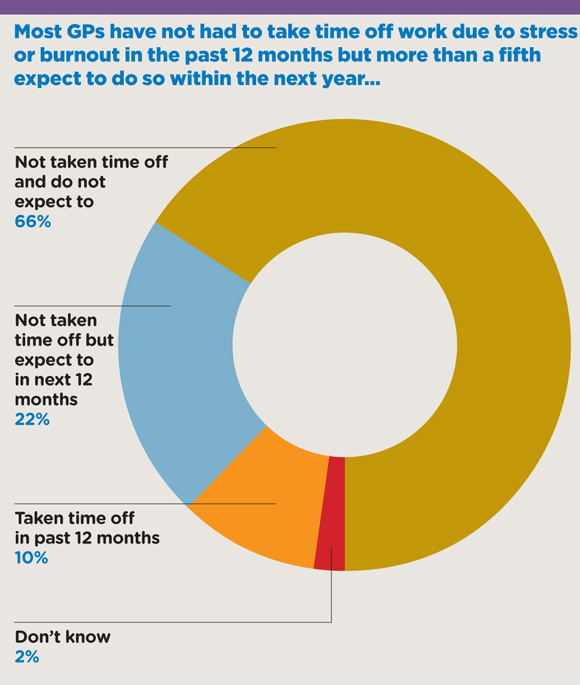
The survey also found that one in 10 GPs has taken time off work in the past 12 months because of stress or burnout, while a further 22% fear it is likely they will do so within the next year.
These figures come after the GP Health confidential counselling service was inundated with GPs suffering with mental health concerns, including stress or depression, or addiction issues.
The service was launched this year following Pulse’s ‘Battling Burnout’ campaign, which highlighted the pressures GPs face from relentless workload, and saw 500 self-referrals within its first four months of operation.
Around 15% of the GPs who responded to Pulse’s survey said they had turned to alcohol, prescription drugs or both to help them ‘deal with work pressures’.
One GP – who wished to remain anonymous – said: ‘I drink a bottle of wine most evenings after work, and often take codeine to help me sleep. I’m also on long-term antidepressants, as are a lot of my colleagues.’
Other respondents had similar stories: ‘I’m more likely to drink a glass of wine on a work night than on a non-work day’; ‘I started self-treating, perhaps stupidly’; ‘I’m on melatonin bought abroad to help sleep’; and ‘I don’t think I could work without fluoxetine’.
A major University of Oxford study, published last year, showed GP workload has increased by 16% since 2007 and patients see their GP 14% more than seven years ago. The researchers said practices had reached ‘saturation point’.
A number of GPs told Pulse how the pressure affects patient care, with many citing the effect on their empathy and commitment to the profession.
Dr Stephen Aras, a GP in West London, said: ‘I care less about me and my career – I have to “care less” or else the pain would be too much to bear.’
Other GPs referred to ‘getting irritated with patients when it is not their fault’, and ‘compassion fatigue’.
It also affects other areas of the job: a few GPs highlight ‘taking more shortcuts’ and ‘a reduced willingness to take on risk’. One said ‘the sheer volume and pressures mean my recordkeeping is awful’.
Exeter GP Dr Kate Dick summed up the message of the survey, saying: ‘Sheer volume of work is making me less sympathetic at the end of the day and after a full day on duty I still have to offer an extended hours routine surgery from 6.30 to 7.30pm for working patients. I am not the best GP I could be at this time.’
Former RCGP chair Professor Clare Gerada, who runs the GP Health service, said: ‘‘It’s worrying that one in 10 doctors go home and use alcohol to relax. That’s high. With prescription drugs, even 6% is a significant number who have expressly gone to their doctor for benzodiazepines and antidepressants to address work-related stress.’
An NHS England spokesperson said: ‘We fully understand GPs are on the front line when it comes to dealing with rising patient demand. This is why we have launched a world-first, nationally funded service to support GPs and GP trainees suffering mental ill health and addiction, while implementing measures to boost the wider primary care workforce and reduce individual GP workload.’
If you are worried about your health, then you are able to access free counselling in England from the GP Health Service. Click here for more details.
data 1 nov2017 580×685

data 2 nov2017 580×1069
data 3 nov2017 580×569
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.












