This site is intended for health professionals only

An initiative in Cheshire focuses on patients with hypertension or COPD. Dr Dan Bunstone, clinical director of the Warrington Innovation Network PCN, explains how it works
This pilot in Warrington, Cheshire, aims to support patients with hypertension or COPD to minimise their risk of hospital admission and significant health events such as heart attack or stroke.
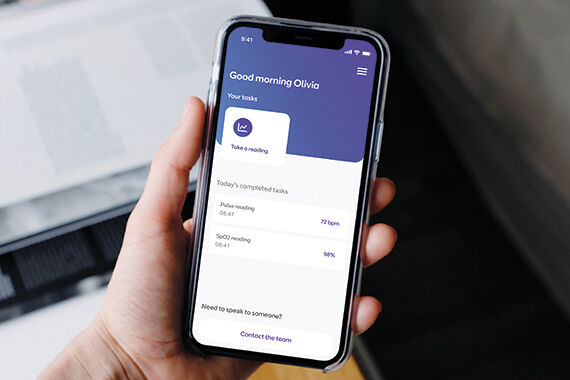
It is jointly funded by our PCN and Etc Health, which is part of the telecoms provider BT Group. Etc Health has created an app for patients to upload clinical data that can be viewed by our clinical teams. This gives us a remote monitoring platform to actively assess, monitor and treat patients. The app is not yet generally available. Our team is helping to refine it and it should be ready for download soon.
Seven practices are involved in the project. We have rolled it out across the whole Warrington Innovation Network (WIN) PCN.
Aims
We knew that the burden of disease would become untenable unless we invested in future health.
In Warrington, respiratory conditions, including COPD exacerbations, are the largest driver of A&E attendances. Up to 47% of COPD patients experience at least one exacerbation per annum and the likelihood of another increases with each occurrence.
By proactively monitoring and holistically managing our COPD patients, we aim to provide increased support when they need it. We can spot when their condition starts to deteriorate – often before they’ve spotted it themselves – enabling rapid treatment and quicker recovery.
Hypertension is a significant and direct risk factor for heart attack and stroke. Optimising our management of the condition is incredibly cost-effective and helps us prevent hundreds of heart attacks and strokes each year across just our integrated care system (ICS).
We know that blood pressure control nationally needs improvement, and Covid-19 has exacerbated this. We aim to identify patients with hypertension who would benefit from closer intervention and risk stratifying. We offer them the Etc Health app, which enables patients to upload details to be viewed by our clinical teams.
Through a combination of holistic and medication changes, we support them to achieve good blood pressure control. The aim is to engage more effectively with patients who previously have been harder to reach, as we can see when readings are submitted and follow up on any gaps. It helps with adherence and goal setting and is a significant driver for behavioural change.
Methods
For both long-term conditions, we are taking a hybrid approach that combines remote care with in-person support as needed.
We use a risk stratification tool created by UCL Partners,1 which is clinically validated and very effective. It enables us to direct care towards the patients who most need it, so care is delivered where it is effective instead of on a ‘fair shares’ basis.
We have also created health kiosks in the seven PCN member surgeries, which were purchased by the PCN using GP transformational funding.
Health kiosks enable patients to take their own blood pressure, pulse and BMI, which then feeds directly to their GP records. This is used as a single-point test to identify patients who may need greater intervention. We run searches to pick up readings submitted that week.
Patients who are flagged are offered the app and their clinical observations are monitored for two weeks.
For COPD, we monitor oxygen saturations and pulse rate. For hypertension, we measure blood pressure and pulse rate.
Our clinical team then monitors the patient inputs. Remote monitoring is incredibly efficient, and we can offer intensive management with micro-interventions. We can see when patients become unwell and react early. We can spot missed readings and remind the patient to upload a new one. And we can ask how medication changes are being tolerated.
Patients are pre-emptively booked into follow-up appointments with a prescribing nurse or a clinical pharmacist so that changes can be made to their medication as necessary. The patient can also have sessions with a healthcare assistant or pharmacy technician, who will work through lifestyle advice.
Outcomes
Over the course of the project, we will see at least 1,000 patients, and we hope to see even more. This will be a mixture of more acute COPD patients and patients with a known diagnosis of hypertension in whom treatment has yet to be fully optimised.
Feedback from patients has been overwhelmingly positive. They love the proactive care and feel safe and supported in their medical condition. For hypertension, we are able to significantly impact our patients’ management. We anticipate that over the next six to 12 months, the project will prevent 10 heart attacks and 20 strokes1 with reduced hospital admissions.
For COPD, we have registered about 100 patients across our PCN who have a diagnosis and are at risk of hospital admission. We have proactively managed their care, supported them to optimise their
health when they feel well, and quickly managed their care when they deteriorate.
Ultimately, this improves quality of life, helps our patients feel supported, and reduces unplanned attendance at both the GP surgery and hospital. We are supporting hospital discharge by preventing the initial admission.
With support from our integrated care board (ICB) team in Warrington, we are using 1,250 oxygen sats machines that the NHS purchased to support Covid management and we aim to increase that number.
Patients input their oxygen saturation readings to be monitored by our clinical team. If readings show deterioration, the clinical team will contact the patient to ensure all is well, and where appropriate will arrange assessment and follow up. Our experience is that early intervention and support of this kind is valued by patients – simply knowing that someone is actively looking after their care is much of the help they need.
We also have Bluetooth-enabled devices for both pulse oximetry and blood pressure, but as we already had the surplus oxygen sats monitors, we wanted to rapidly mobilise them for our patients.
We’ve also collaborated with the local authority to provide the additional support of social prescribers and signposting, which has proved very effective. And we are supporting COPD patients who have been identified as experiencing fuel poverty, tackling the problem now before we hit winter 2023.
Also, we’ll have made a start on the long process of changing the culture of health in our PCN. Instead of patients seeking care when they feel unwell, they will be contacted before they become ill. This is the power of collaborative working and digital technology.
The NHS needs to balance the problem of in-year demand with supporting the future, which is one of the focuses of this project. By supporting COPD patients, we increase efficiencies by preventing A&E admissions. By supporting blood pressure management, we prevent heart attacks and strokes.
The ultimate aim is that our patients will always have access to the Etc Health app, to track their results and get support for improving health behaviours. The partnership with Etc Health is also allowing us to test and innovate digital products.
We hope to increase the breadth and depth of the project by sharing ideas with the other PCNs and supporting a full rollout across the other PCNs in Warrington.
We also hope to increase the number of long-term conditions we can support. Heart failure and diabetes are the two we are considering next, and possibly also frailty.
Dr Dan Bunstone is clinical director of Warrington Innovation Network (WIN) PCN, clinical advisor at Etc Health, and chair of the NHS Confederation’s PCN data and digital design group
Reference

Register today to receive weekly newsletters and a free copy of Pulse PCN with Pulse magazine
Sign up now